When you look at a CT scan, you expect to see a perfect, detailed map of the inside of the human body. But sometimes, the image has flaws—streaks, shadows, or strange patterns that aren't actually part of the patient's anatomy. These are CT artifacts.
Think of them like static on an old TV or a lens flare in a photograph. They're visual distortions that can get in the way, making it harder to see what's really going on. These aren't just random glitches; they're systematic errors that can obscure, mimic, or completely hide crucial clinical information, sometimes even leading to a misdiagnosis.
What Are Artifacts in Computed Tomography?
Computed tomography (CT) is a cornerstone of modern radiology services, giving us incredible cross-sectional views of the body. The process, however, is incredibly complex. Any hiccup—whether from the patient, the scanner's hardware, or the physics of how X-rays travel through tissue—can introduce errors. These errors show up on the final image as artifacts.
An artifact can take many forms. You might see streaks radiating from a dense object, dark bands, bizarre rings, or just a general graininess that makes the image look noisy. Each type of artifact is a clue, pointing back to a specific cause.
Why Recognizing Artifacts Is So Important
For radiologists and CT technologists, spotting and understanding artifacts is a non-negotiable skill. It's not just about getting a "pretty picture"; it has serious clinical implications.
- Mimicking Disease: Some artifacts are master impersonators. A common streak artifact in the brain, for instance, can look frighteningly similar to a bleed.
- Obscuring Pathology: A dense metal implant, like a hip replacement, can cast long, dark shadows that completely blot out the surrounding tissue, potentially hiding a tumor or fracture.
- Reducing Diagnostic Confidence: An image filled with artifacts erodes a radiologist's confidence. This uncertainty can lead to inconclusive reports and may force the patient to undergo additional, often unnecessary, scans.
Artifacts have been a challenge since CT scanners first hit the market in the 1970s. Even with today's sophisticated technology, it's estimated that 10-15% of CT images still show noticeable artifacts. Modern reduction techniques have made a big difference, often cutting their severity by 40-60%. You can learn more about the evolution of CT device technology on databridgemarketresearch.com.
Getting to the root of an artifact is the first step in fixing it. By figuring out where it came from—the patient, the scanner, or the physics of the imaging process—we can use specific strategies to clean up the image and get a clear, accurate diagnosis.
To get a better handle on this, let's break down the most common types of artifacts you're likely to encounter.
Common CT Artifact Categories at a Glance
This table provides a quick cheat sheet for the main categories of artifacts, their causes, and what they typically look like on a scan.
| Artifact Category | Common Cause | Visual Appearance |
|---|---|---|
| Physics-Based | The physical interaction of X-rays with tissue. | Streaks, dark bands, cupping (center of image appears darker). |
| Patient-Based | Patient movement or metallic objects in/on the patient. | Blurring, ghosting, severe streaks radiating from metal. |
| Scanner-Based | Hardware malfunctions or calibration issues. | Rings, concentric circles, lines across the image. |
| Helical & Cone-Beam | Specific to the geometry of multi-slice helical scanners. | Windmill-like or cone-shaped patterns, especially at the edges. |
Each of these categories contains several specific artifacts, which we'll dive into next. Understanding them is key to mastering CT image quality.
Why Physics-Based Artifacts Appear
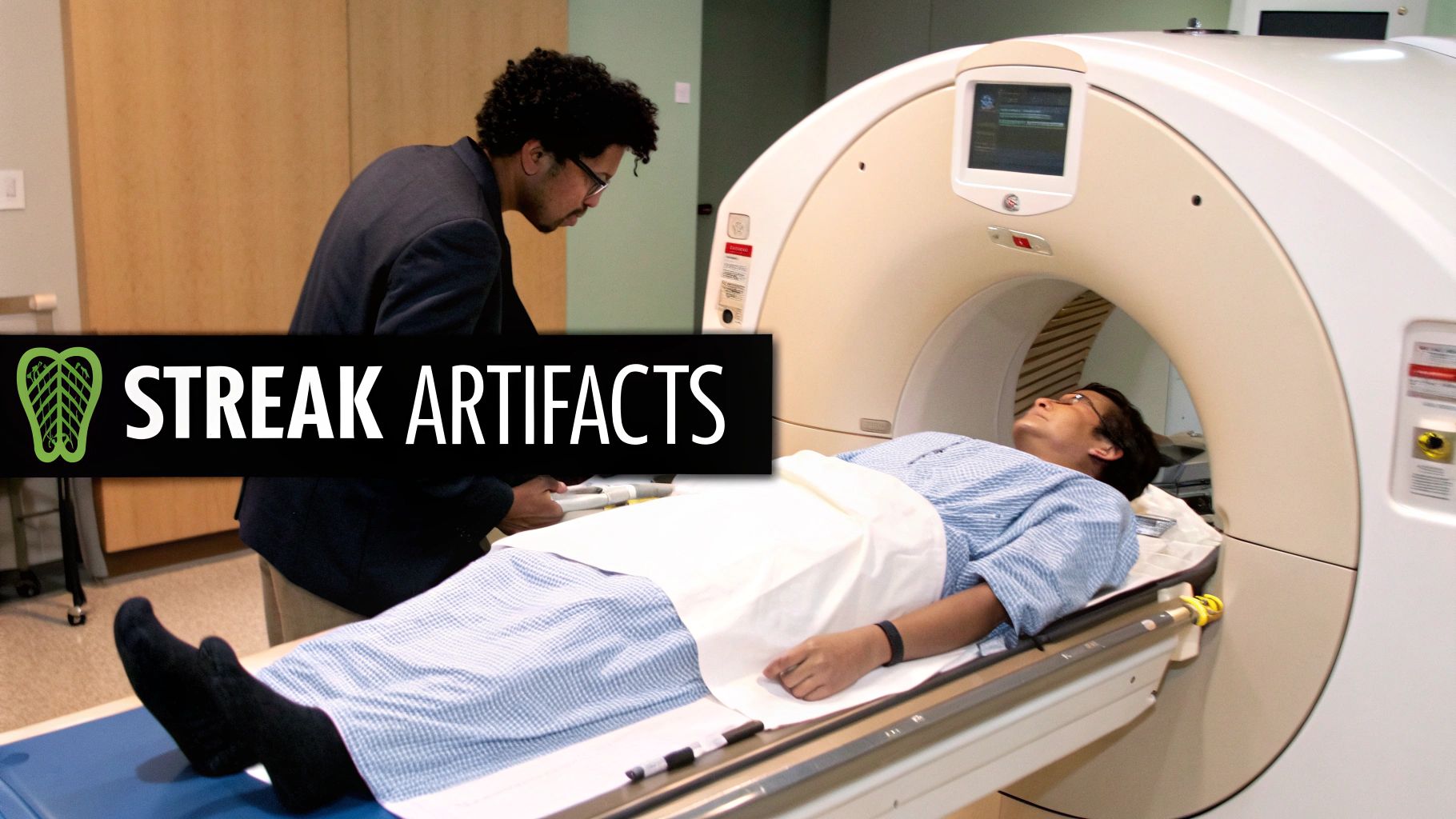
At its core, a CT scanner is a sophisticated physics machine. It fires a beam of X-rays through the body, measures how those X-rays get weakened, and then uses some seriously complex math to reconstruct an image. But the very laws of physics that make this incredible technology work can also be the source of errors.
These physics-based artifacts aren't the result of a broken scanner or a fidgety patient. They are built into the fundamental interaction between X-rays and human tissue.
Think of it like recording audio in a room with a natural echo. You can’t just "turn off" the echo; it's a property of the room itself. Instead, you learn to work with it, using specific techniques to minimize its impact on the final recording. The same principle applies here. By getting a handle on the physics behind these image distortions, we can learn to anticipate, recognize, and ultimately correct for them.
Let's break down three of the most common physics-based artifacts you'll encounter.
Demystifying Beam Hardening
Imagine you’re sifting for gold. Your sifter has a mesh that lets fine sand fall through but catches the larger, heavier nuggets. This is a perfect analogy for beam hardening.
The X-ray beam from a CT scanner isn't one single energy. It's actually a spectrum, containing a mix of low-energy ("soft") and high-energy ("hard") X-rays. As this beam travels through the body, the softer, weaker X-rays are easily absorbed by tissues like skin and muscle.
This process effectively filters out the weaklings, leaving a beam that is, on average, "harder" and more powerful than when it started. The scanner's standard reconstruction math doesn't fully account for this shift in energy, which leads to some very predictable visual artifacts.
What Beam Hardening Looks Like:
- Cupping Artifact: In an image of a fairly uniform structure, like the brain, the center appears darker than the edges. This gives it a distinct "cupped" or dish-like look.
- Streaks and Dark Bands: When the beam has to pass between two extremely dense objects, like the petrous bones of the skull, it gets severely hardened. This creates dark streaks and bands between them, which can easily hide the anatomy you’re trying to see.
This is without a doubt one of the most common artifacts in CT, and modern scanners rely on specialized correction software to tackle it.
Understanding Partial Volume Averaging
Ever tried taking a picture with a low-resolution camera? Imagine one of its huge pixels lands half on a black line and half on the white wall behind it. The camera has to make a choice, so it averages the two, and the pixel becomes gray. The sharp edge is gone, replaced by a blur.
That’s the essence of the partial volume averaging artifact. A CT image is built from tiny 3D cubes of data called voxels. If a single voxel happens to contain two different tissue types—say, a small lung nodule and the surrounding air-filled lung—the scanner averages their densities together.
The result is a single, blended value for that entire voxel. This averaging can either completely obscure tiny structures or make the edges of larger objects look fuzzy and ill-defined.
The partial volume effect gets worse when an object is smaller than the CT slice is thick. For example, a 4 mm lesion might show up clearly on a 1 mm slice, but it could be completely blurred into obscurity and missed on a thicker 5 mm slice.
This is precisely why choosing the right slice thickness is such a critical decision for technologists, especially when the goal is to find small pathologies like early-stage tumors or hairline fractures.
Explaining Photon Starvation
If you’ve ever taken a photo in a pitch-dark room without a flash, you know the result: a grainy, noisy mess where details are lost in a sea of speckles. This happens because the camera's sensor didn't get enough light—enough photons—to build a clean image.
Photon starvation is the exact same problem, just with X-ray photons. It happens when the X-ray beam has to punch through an incredibly dense or wide part of the body, like the shoulders or the hips of a larger patient. These areas absorb so many of the X-rays that only a trickle of photons makes it to the detectors on the other side.
This severe lack of signal creates a huge amount of statistical noise in the data, resulting in images that look horribly streaky and grainy.
Common Scenarios for Photon Starvation:
- Scanning the Shoulders: The combination of dense bone and the sheer width of the shoulder girdle can stop a massive number of X-rays, causing nasty streaking across the upper chest and lower neck.
- Abdominal Scans in Bariatric Patients: A larger abdomen naturally attenuates more of the X-ray beam, making it much more likely to produce noisy, low-quality images.
Technologists can fight photon starvation by increasing the radiation dose (mA), but this always has to be balanced against patient safety. Thankfully, modern scanners now employ adaptive filtering and iterative reconstruction algorithms designed specifically to clean up the noise from these low-signal situations, helping to preserve diagnostic quality while keeping the dose as low as reasonably achievable.
Handling Patient-Related Artifacts
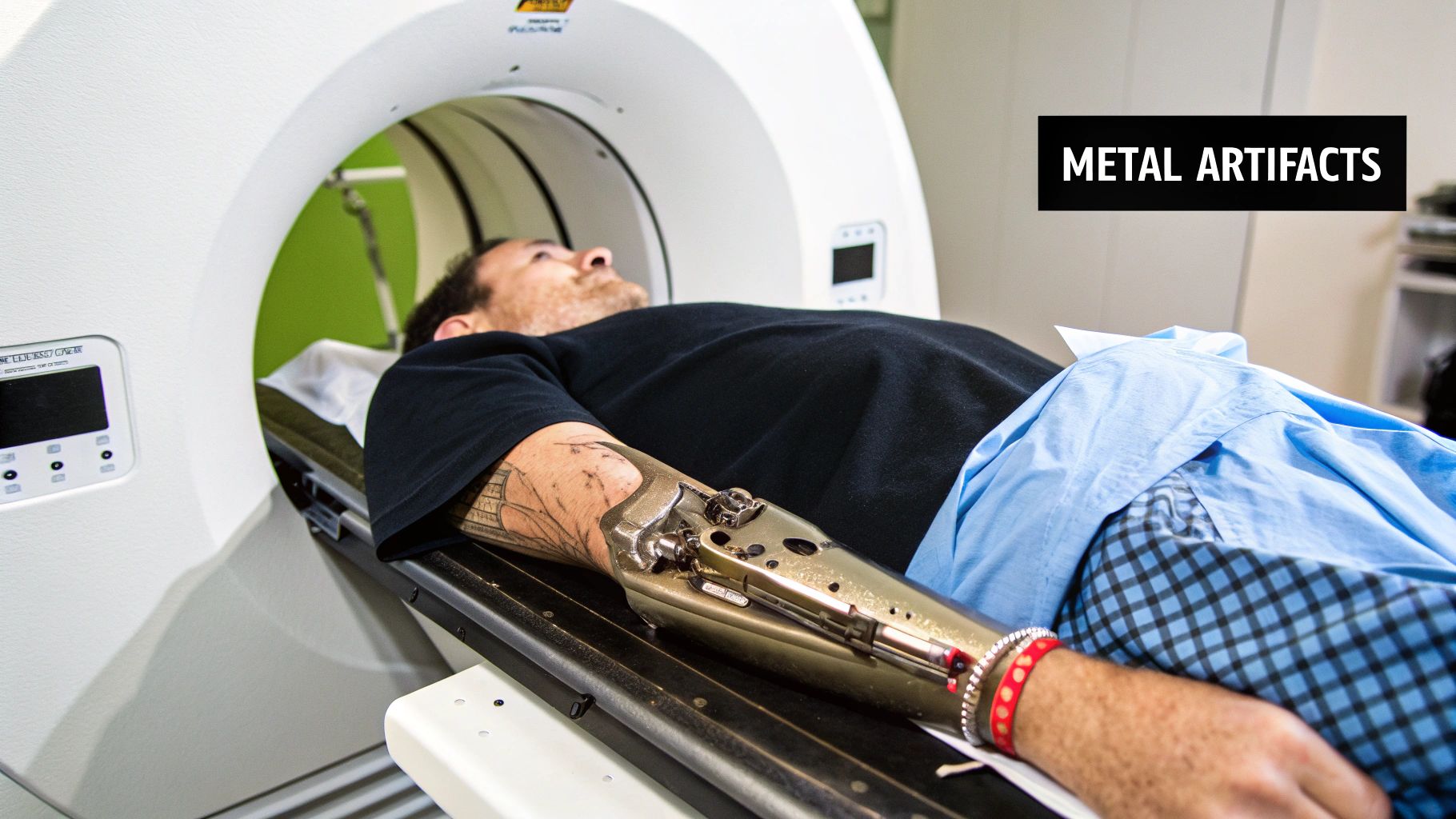
While scanner physics and hardware can cause their share of problems, some of the trickiest artifacts to deal with come directly from the patient. We call these patient-related artifacts, and they pop up because the human body rarely cooperates with the perfectly still, ideal conditions that a CT scanner’s software expects.
Think about it: a CT scanner is essentially taking hundreds of lightning-fast pictures from every angle to build one detailed 3D model. If the person being scanned moves, even just a little, the final image gets blurry and misaligned. Getting a handle on these artifacts is a huge part of a CT technologist's daily job, blending great patient communication with solid technical know-how.
Tackling Motion Artifacts
Movement is, without a doubt, the most common patient-related headache. If you've ever tried to take a sharp photo of a toddler who won't sit still, you already understand the core problem. Any movement during the scan creates motion artifacts, which can smear the image and hide the very details a radiologist needs to see.
This motion generally falls into two buckets.
Voluntary Motion
This is any movement the patient has control over. Things like:
- Breathing during a chest or abdomen scan.
- Swallowing when we're trying to get a clear look at the neck.
- Just fidgeting or shifting because of anxiety or being uncomfortable on the table.
Involuntary Motion
Then you have the movements the patient can't do anything about. These are the body's automatic functions:
- The constant, rhythmic beat of the heart.
- The movement of the bowels, which we call peristalsis.
- The pulsing of major blood vessels.
Whether big or small, these movements feed inconsistent information to the scanner's detectors. The reconstruction software then has a tough time piecing it all together, resulting in streaks, blurs, and a "ghosting" effect where you see double outlines of organs.
The first line of defense is simple: clear communication. A technologist coaching a patient through a breath-hold can work wonders. For involuntary motion, especially with the heart, we use more advanced tricks like cardiac gating to time the scan perfectly with the heartbeat, effectively freezing it in motion.
The Challenge of Metallic Artifacts
Another major source of patient-related artifacts comes from high-density materials inside the body. Metallic artifacts are the dramatic distortions caused by things like dental fillings, prosthetic hips, surgical clips, or screws from a spinal fusion. These objects are so dense they stop nearly all X-rays in their tracks, a phenomenon called extreme beam hardening.
The scanner's detectors sitting behind that piece of metal get almost no X-ray signal, so the system sees a black hole of missing information. The reconstruction algorithm does its best to fill in the blanks, but the result is usually a mess.
What Metallic Artifacts Look Like
These are some of the most obvious and disruptive artifacts you'll see. They typically show up as intense bright and dark streaks shooting out from the metal object like a starburst. They can also cast huge dark "shadows" that completely hide nearby tissues, making a diagnosis in that area impossible.
The clinical impact here is massive. Artifacts from implants like dental work or hip replacements show up in an estimated 10-20% of abdominal and pelvic CTs in many countries. This kind of image degradation is a key reason why roughly 5-12% of all CT scans have to be repeated, which drives up healthcare costs and gives patients unnecessary radiation exposure. You can dig deeper into the CT scanner market data on fortunebusinessinsights.com.
Modern Solutions for Metal Artifacts
Thankfully, we aren't just stuck with this problem anymore. Modern CT scanners come loaded with specialized software called Metal Artifact Reduction (MAR) algorithms.
MAR is incredibly smart software that goes back and cleans up the corrupted data. Here’s a quick look at how it works:
- Find the Metal: The algorithm first scans the data to pinpoint the exact location of the metallic object.
- Fill in the Gaps: Using sophisticated models, it intelligently estimates what the data should have looked like in the areas blacked out by the metal.
- Rebuild the Image: Finally, it swaps the messy, streaky data with its corrected estimates and reconstructs a brand-new, much cleaner image.
These algorithms are game-changers. They can drastically cut down on the streaking and shadows, often saving an otherwise useless scan. This is vital when we need to check the area around a joint replacement for an infection or when planning radiation therapy for a cancer patient who has surgical clips in the way.
When the Scanner is the Culprit
Sometimes, the phantom in the image isn't a physical quirk or a patient's movement—it's a ghost in the machine. These are scanner-based artifacts, and they point directly to a problem with the CT hardware or its calibration.
Think of it like a single dead pixel on your camera sensor. No matter what photo you take, that tiny flaw will appear in the exact same spot. Scanner-based artifacts are just like that. They produce consistent, recognizable patterns that can often be traced back to a specific faulty component.
The good news? Unlike random patient motion, these issues are predictable and repeatable, which makes them much easier to diagnose. Catching them early is the whole game, and that's where the sharp eyes of medical physicists and service engineers come in.
The Tell-Tale Ring Artifact
One of the most classic scanner-based issues is the ring artifact. It looks exactly like it sounds: one or more thin, perfect circles layered over the image, almost as if drawn with a compass.
These rings are almost exclusively found in third-generation CT scanners, where the detector array rotates right along with the X-ray tube. The problem stems from a single detector element that's gone rogue.
Imagine one tiny detector in the array is just a little "off"—maybe it's not as sensitive as its neighbors, or its calibration has drifted. As the gantry spins a full 360 degrees, that one faulty detector maps out a perfect circle in the data. The reconstruction software, not knowing any better, sees this consistently bad signal and treats it as a real anatomical structure, creating a ring.
A ring artifact is a clear distress signal from the scanner. It’s not an interpretation puzzle; it's a direct sign of a hardware problem that needs immediate recalibration or detector replacement.
Artifacts from Modern Scan Geometries
As CT technology got faster and more powerful, new types of scanner-related artifacts came along for the ride. Modern multi-detector CT (MDCT) scanners use a wide, cone-shaped X-ray beam to capture huge volumes of data in a single helical (spiral) pass. This is incredibly efficient, but the complex geometry introduces its own challenges.
-
Cone Beam Artifacts: These tend to pop up at the edges of the image, corresponding to the outermost detector rows where the X-ray beam is at its widest angle. This can create a distinct "windmill" or star-like pattern, especially when scanning through areas with big density differences.
-
Helical Artifacts: When you scan a long stretch of the body in a spiral, objects that are sharply angled to the scan plane can look distorted or blurred. It's a type of distortion you just wouldn't see in a conventional slice-by-slice axial scan.
While these artifacts are baked into the design of modern scanners, engineers have developed incredibly sophisticated reconstruction algorithms specifically to correct for these geometric hiccups before they ever reach the final image.
Why Maintenance and Calibration Are Everything
The most important thing to remember about scanner-based artifacts in computed tomography is that they are almost always preventable. These aren't random flukes; they're symptoms of a system that's drifted out of tune.
This is exactly why routine quality control and preventative maintenance are non-negotiable in radiology. Medical physicists run a tight ship, performing daily, weekly, and annual checks to ensure every last component is working exactly as it should.
Key Maintenance Procedures Include:
- Detector Calibration: Technologists run regular calibration scans, often called "air scans," to make sure every single detector element is responding uniformly.
- Phantom Scans: They scan special objects called phantoms, which have known densities. This lets them check for image uniformity, noise, and sneaky artifacts like rings before they show up on a patient scan.
- Mechanical Checks: Service engineers ensure the gantry's rotation is perfectly smooth and aligned to prevent any geometric warping of the images.
This strict regimen is the first line of defense, catching tiny performance drifts long before they can grow into a problem that might affect a patient's diagnosis.
Modern Solutions for Artifact Reduction
Spotting an artifact is one thing, but getting rid of it is a whole different ball game. As the demand for clearer, more precise imaging grows, manufacturers and technologists are leaning on some seriously powerful software and hardware to get the job done. These aren't just minor adjustments; they represent a fundamental shift in how we acquire and process CT data.
Instead of just shrugging our shoulders and accepting artifacts as part of the deal, these modern methods actively work to prevent them from ever forming or erase them after the fact. Let's dig into three key technologies leading the charge: iterative reconstruction, dual-energy CT, and the ever-growing role of artificial intelligence. Each brings a unique playbook to the table for overcoming the classic pitfalls of CT imaging.
The Art of Iterative Reconstruction
For decades, the go-to method for building a CT image was a process called filtered back projection (FBP). It's fast and it works, but FBP is notorious for creating noise and artifacts, especially when you're trying to keep the radiation dose low. Iterative Reconstruction (IR) is the smarter, more refined alternative.
Picture two sculptors. The FBP sculptor glances at a model, then carves a statue in one quick, single pass. The IR sculptor, on the other hand, starts with a rough shape, compares it to the model, spots the mistakes, and makes corrections. They repeat this cycle—carve, compare, correct—over and over, getting closer to a perfect replica with each loop.
That's exactly how IR works. It generates an initial image, checks it against the raw scan data, identifies the differences (the "errors," or artifacts), and then refines the image. This loop continues until the final image is a near-perfect match to the source data, dramatically cutting down on noise and other distortions.
By 2024, iterative reconstruction techniques are integrated into over 80% of newly sold CT scanners, a clear sign of their clinical impact. This is happening as the global CT market, driven by the need for better diagnostics, is expected to top USD 12 billion by 2032. You can learn more about these market dynamics on maximizemarketresearch.com.
The best part? This approach allows for significantly lower radiation doses without giving up image quality, which is a massive win for patient safety.
Using Two Energies Instead of One
Another powerful weapon in the fight against artifacts, especially those from beam hardening and tricky materials, is Dual-Energy CT (DECT). A standard scanner blasts a patient with an X-ray beam that has a single, broad energy spectrum. A DECT scanner, however, uses two different X-ray energy levels at the same time.
Think of it like looking at the world with your regular vision, then switching to an infrared camera. Each view reveals different information. DECT does something similar by analyzing how materials like bone, soft tissue, and contrast dye absorb the high- and low-energy X-rays differently. This two-layered approach allows the system to:
- Better Differentiate Tissues: It can accurately tell the difference between materials with similar densities, like iodine contrast and bone.
- Create "Virtual" Images: It can generate images that look as if they were taken with a single-energy beam, which effectively cancels out beam hardening artifacts.
- Reduce Metal Artifacts: The extra data helps algorithms better understand what's going on around metallic implants, which is a big boost for metal artifact reduction software.
At the end of the day, DECT delivers a much richer dataset. This gives radiologists more information to work with and produces images that are inherently more resistant to certain physics-based artifacts.
The Rise of Artificial Intelligence in Artifact Correction
The newest frontier in this battle is Artificial Intelligence (AI), specifically a technique called deep learning. You can train AI models on massive libraries of CT images—some full of artifacts, others nearly perfect—to teach them exactly what an artifact looks like and, more importantly, how to get rid of it.
Imagine a master photo editor who has spent a lifetime retouching images. They can spot a stray hair or a dust speck instantly and make it disappear without a trace. A well-trained deep learning model does the same for artifacts in computed tomography. It recognizes the unique patterns of streaks, noise, and rings, then intelligently subtracts them from the image while leaving the true anatomy untouched. This is a game-changer.
- Speed: AI-powered correction happens in seconds, fitting seamlessly into a busy clinic's workflow.
- Versatility: You can train a single AI model to spot and fix multiple types of artifacts all at once.
- Quality Improvement: AI can often rescue scans that would have been thrown out as non-diagnostic because of severe artifacts.
To put these advancements in perspective, let's compare how traditional methods stack up against these newer technologies.
Comparing Artifact Reduction Techniques
This table highlights the evolution from basic filtering to the sophisticated, data-driven approaches we have today. Each step forward offers a more targeted and effective way to clean up images.
| Technique | Primary Artifacts Addressed | Mechanism | Clinical Advantage |
|---|---|---|---|
| Traditional (FBP) | General Noise, Streaks | Mathematical filtering of projection data before reconstruction. | Fast and computationally simple, the historical standard. |
| Iterative Reconstruction (IR) | Noise, Low-Dose Artifacts | Cyclical process of comparing a reconstructed image to raw data and correcting errors. | Enables significant radiation dose reduction with superior image quality. |
| Dual-Energy CT (DECT) | Beam Hardening, Material-Specific | Acquires data at two energy levels to differentiate materials based on their atomic number. | Improves tissue characterization and removes artifacts from dense materials. |
| Artificial Intelligence (AI) | Wide Range (Noise, Metal, Motion) | Deep learning models trained to recognize and remove artifact patterns from images. | Highly effective and versatile; can salvage otherwise unusable scans. |
While older methods laid the groundwork, it's clear that modern technologies like IR, DECT, and AI provide a much more robust toolkit for achieving diagnostic clarity.
The infographic below shows just how big of a leap we've made, especially with deep learning.

The data speaks for itself. We've seen a massive jump in our ability to clean up CT images, with deep learning leading the pack. As these technologies get even better, they promise a future where a crystal-clear, diagnostically perfect image is the standard, not the exception.
Frequently Asked Questions About CT Artifacts
Even after digging into the technical side of CT artifacts, you might still have some practical questions about what they mean in the real world. This section tackles some of the most common queries we hear, closing the loop between the physics of image distortion and its impact in a clinical setting for patients and medical teams alike.
Can CT Artifacts Lead to a Wrong Diagnosis?
Absolutely, and that’s precisely why identifying them is so important. These visual glitches can do one of two things: they can either mimic a real medical problem or completely obscure one, both of which can lead to a serious misdiagnosis.
Think about it this way: heavy streak artifacts in the brain could easily be mistaken for a hemorrhage. On the other hand, even a tiny bit of motion during an abdominal scan could blur the edges of a small tumor on the liver, causing a radiologist to miss it entirely. The stakes are incredibly high.
When an artifact corrupts a key diagnostic area, the radiologist has to make a tough call. Often, the only safe option is to repeat the scan, this time with settings adjusted specifically to avoid the artifact that showed up the first time.
This is where the expertise of a seasoned radiologist really shines. They need to be able to tell the difference between a genuine medical finding and a "ghost" in the machine.
Are Some People More Prone to Causing Artifacts?
Yes, certain patient-specific factors definitely increase the chances of artifacts appearing on a scan. Metal inside the body is probably the most common cause.
- Metallic Implants: Anyone with joint replacements, pacemakers, surgical clips, or even extensive dental work is a prime candidate for creating major metal artifacts.
- Patient Motion: It’s tough to stay perfectly still, especially if you're in pain, feeling anxious, or have a condition like Parkinson's. Any movement can create blurry, streaky images.
- Body Size: For larger patients, the X-ray beam has more tissue to travel through, which weakens it. This can cause photon starvation, an artifact that makes the final image look noisy or grainy.
Skilled CT technologists know to look for these potential issues ahead of time and will adjust their approach to get the clearest scan possible.
Whose Job Is It to Deal with Artifacts?
It’s really a team effort between the CT technologist and the radiologist. Each has a crucial role to play in spotting and managing these image distortions.
The technologist is on the front line. It's their job to:
- Give clear instructions to the patient, like when to hold their breath.
- Use cushions or other devices to help the patient stay comfortable and still.
- Choose the right scan settings based on the patient's body and the reason for the scan.
The radiologist is the final interpreter. They have to spot any artifacts in the images, figure out what caused them, and decide if the scan is still good enough to make an accurate diagnosis. If the image quality is too compromised, the radiologist makes the final call on whether to repeat the scan or if they can safely make a diagnosis with what they have.
At PYCAD, we're building intelligent AI tools designed to help medical professionals spot and minimize artifacts. Our goal is to ensure they have the cleanest images possible to make life-saving diagnoses with confidence. Our models fit right into existing hospital workflows, making medical imaging more accurate and efficient.






