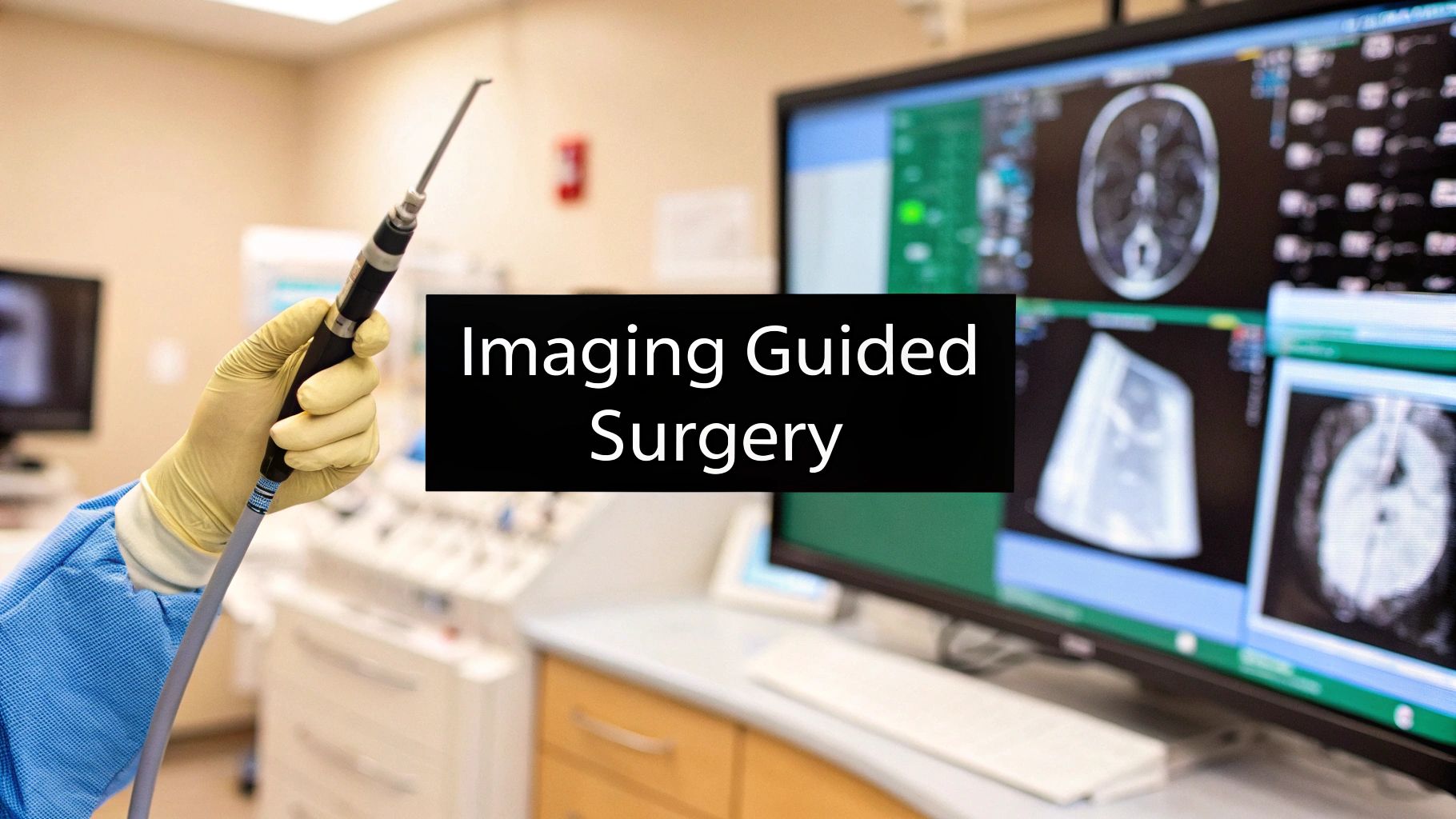
Imagine a surgeon having a GPS for the human body, one that allows them to navigate the most delicate and complex anatomical structures with absolute precision. That's the essence of imaging guided surgery (IGS). It's a method that takes pre-operative scans and turns them into a live, interactive map right inside the operating room.
In a way, it gives surgeons a form of 'x-ray vision,' making today's procedures fundamentally safer and more effective.
What Is Imaging Guided Surgery
At its core, imaging guided surgery is all about merging high-quality diagnostic images with the physical reality of an operation. The best way to think about it is like the navigation system in your car. Before you start a long drive, you might look at a map to get the lay of the land—that's your pre-operative scan. Once you're on the road, your GPS shows your car's exact position on that map in real-time, pointing out every turn.
IGS operates on the very same principle. Surgeons start with detailed patient scans, like a CT or MRI, which are used to build a precise 3D model of the target anatomy. Once in the OR, a sophisticated system of cameras and trackers monitors the exact position of the surgical instruments. The system then overlays the real-time location of those tools directly onto the 3D model displayed on a screen.
The Power of Real-Time Navigation
This seamless integration provides the surgical team with a live, dynamic view of where their instruments are relative to critical structures—things like major blood vessels, delicate nerves, or the precise margins of a tumor. This isn't just a static picture; it's an active guide that updates with every single movement.
This constant feedback loop allows for incredibly meticulous planning and execution. The whole point is to boost surgical precision, minimize any damage to surrounding healthy tissue, and ultimately improve the safety and success of the entire procedure.
The image below really captures this idea of guided precision, showing how a surgeon uses a 3D scan on a monitor to inform every action they take during the procedure.
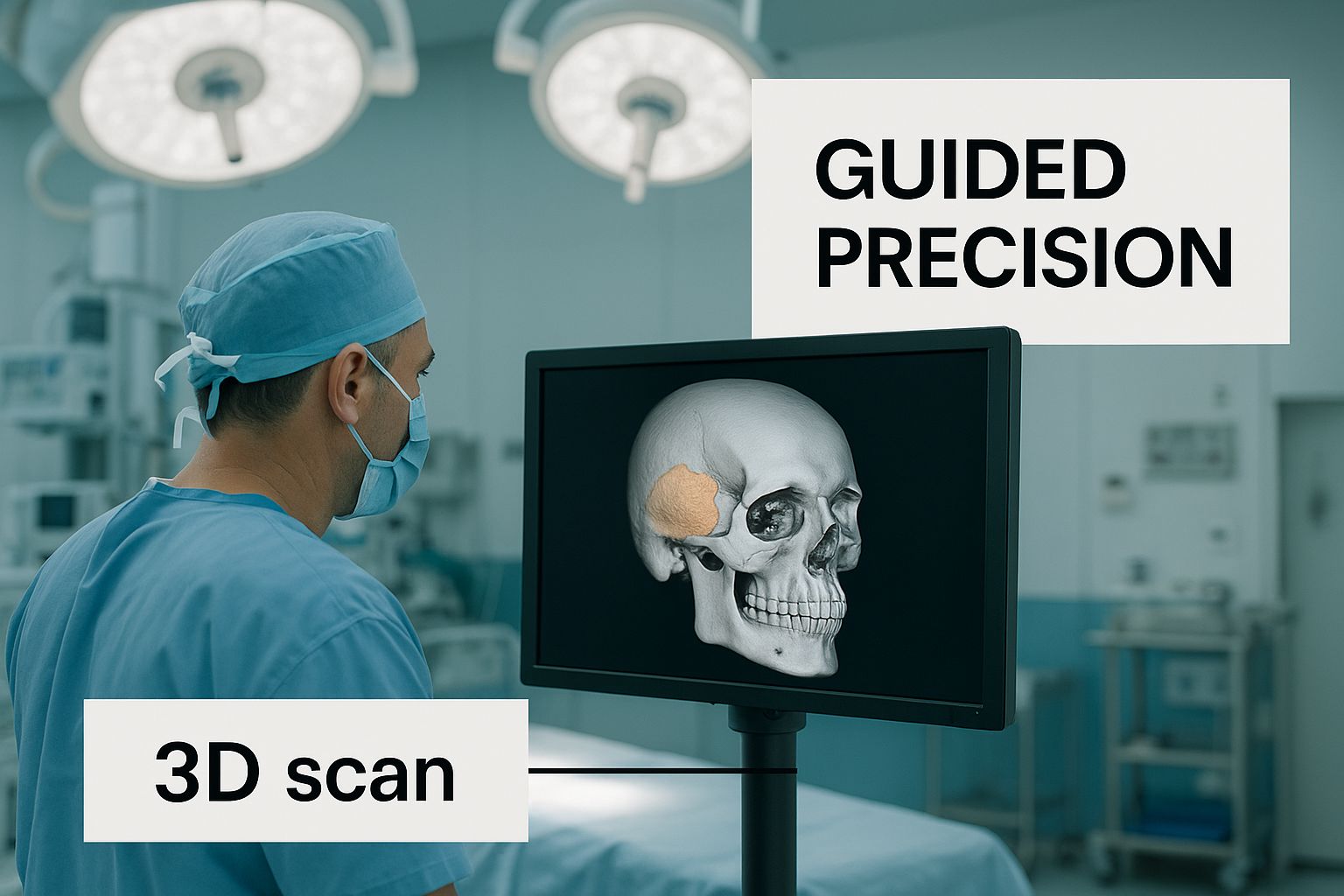
As you can see, the central concept of IGS is blending digital information with physical action to reach a much higher standard of surgical accuracy.
The Technology Behind the System
An IGS system isn't one single piece of equipment but rather a collection of advanced technologies all working in perfect harmony. Each piece has a critical job to do in creating that seamless navigation experience for the surgeon. To truly understand how it all comes together, it helps to break down the main parts.
Core Components of an Imaging Guided Surgery System
A breakdown of the essential technologies that enable real-time surgical navigation.
| Component | Function & Analogy | Common Technologies Used |
|---|---|---|
| Imaging Modalities | The Mapmaker. This is what creates the detailed anatomical "map" before or during the surgery. | CT Scanners, MRI Machines, 3D C-arms, Ultrasound |
| Tracking System | The Satellite Network. It pinpoints the exact location of the patient and surgical tools in 3D space. | Optical (Infrared Cameras), Electromagnetic (EM) Field Generators |
| Computer Workstation | The Central Processor. This is the "brain" that merges the map and the satellite data, displaying it for the user. | High-performance computer with specialized software |
| Tracked Instruments | The GPS Transponders. These are surgical tools fitted with markers so the tracking system can "see" them. | Instruments with attached reflective markers or EM sensors |
By bringing these elements together, the system provides a clear, real-time view that helps guide the surgeon's hand.
This technology represents a fundamental shift in how surgery is performed. It moves surgeons beyond relying solely on anatomical knowledge and the feel of their instruments. Instead, it adds a powerful layer of data-driven insight, empowering them to tackle complex procedures with a level of confidence and accuracy that was once unimaginable.
This leap forward is what enables less invasive techniques, helps reduce complication rates, and often gets patients back on their feet faster, marking a true milestone in modern medicine.
The Journey from Open Surgery to Surgical Navigation
To really get a feel for the incredible accuracy of modern imaging guided surgery, you have to look back at how things used to be done. For centuries, surgery was all about the "open" approach. It relied on a surgeon's deep knowledge of human anatomy, a steady hand, and the ability to see the surgical field directly through a large incision.
This traditional method was both an art and a science. Surgeons used their sense of touch to identify what felt wrong, their eyes to navigate a maze of tissues, and their extensive training to steer clear of vital structures. While this approach saved countless lives, it had its downsides. Large incisions naturally mean more trauma to the body, which leads to more post-operative pain, a greater risk of infection, and a much longer road to recovery. It was a constant balancing act between getting the access needed and minimizing collateral damage.
A New Way of Seeing
The first crack in this old paradigm didn't happen in an operating room, but in a physics lab. When Wilhelm Röntgen discovered the X-ray in 1895, it was the first time we could peek inside the human body without making a cut. All of a sudden, doctors could see broken bones and foreign objects, which completely changed the game for diagnostics. Still, these were just flat, static shadows—great for a diagnosis, but not something you could use to guide a scalpel in real time.
The real jump happened much later, with the arrival of more sophisticated imaging. The invention of Computed Tomography (CT) in the 1970s and Magnetic Resonance Imaging (MRI) in the 1980s was a massive leap forward. For the first time, surgeons had access to incredibly detailed, cross-sectional views of the body.
These tools gave surgeons a detailed "map" before they even entered the operating room. They could pinpoint a tumor's exact location and size or meticulously plan the perfect trajectory for placing a screw in a fractured bone. But a big problem remained: the map was still completely separate from the actual "territory"—the patient lying on the operating table.
Connecting the Map to the Patient
The final, crucial piece of the puzzle was building a bridge between the digital scans and the physical patient. The challenge was to track the surgeon's tools in real time and show their precise location on those pre-operative images. Think of it like a GPS for surgery, placing a "You Are Here" dot on that detailed anatomical map.
This is where surgeons and engineers began working together, developing tracking systems that used infrared cameras or electromagnetic fields. By attaching special markers to the surgical instruments and the patient, these systems could pinpoint a tool's position and angle with sub-millimeter accuracy. This data was then fed into a computer, which overlaid it directly onto the patient's CT or MRI scans.
This fusion of high-resolution imaging with real-time instrument tracking is the heart and soul of surgical navigation. It elevated surgery from a practice based on feel and estimation to one guided by precise, verifiable data.
This shift didn't just refine old procedures; it made entirely new ones possible. With imaging guided surgery, surgeons could now confidently navigate through tiny incisions, knowing their exact position every step of the way. The evolution from the large, open incision to the minimally invasive, data-guided procedure represents a fundamental change in how we think about surgery—one that has radically improved patient safety, slashed recovery times, and redefined the boundaries of what can be achieved in the operating room.
The Surgeon's High-Tech Eyes: Key Imaging Technologies in the OR
To make imaging guided surgery a reality, surgeons have an incredible toolkit of visualization technologies at their disposal. Each one gives them a unique window into the human body, and the right tool is chosen based on the specific job at hand. It’s a lot like a master craftsman selecting a specific chisel for a delicate carving—you need the perfect instrument for the task.
This surgical toolkit isn’t just expanding; it’s fueling a massive boom in medical technology. The global market for these devices was valued at around USD 8.5 billion and is expected to rocket to USD 21.4 billion by 2035. This incredible growth shows just how much modern medicine relies on these precise, minimally invasive methods. You can dig deeper into the data on this market expansion and what's driving it.
So, let's look at the core technologies that act as the eyes of today's surgeon. Each has its own strengths, making it indispensable for different types of procedures.
Computed Tomography: The Master of Bony Detail
When it comes to surgeries involving bone and other hard structures, Computed Tomography (CT) is the undisputed workhorse. A CT scanner is a sophisticated machine that takes a series of X-ray images from countless angles. A computer then gets to work, digitally stitching them together to create highly detailed, cross-sectional "slices" that form a complete 3D model of the patient's anatomy.
Think of it this way: a single X-ray is like looking at the shadow of an object. You get a general idea of its shape, but not the full picture. A CT scan, on the other hand, is like having hundreds of shadows from every conceivable angle, allowing you to build a perfect digital replica.
This level of detail is non-negotiable for:
- Orthopedic Surgery: In complex spinal fusions or joint replacements, surgeons use CT guidance to place screws and implants with pinpoint accuracy, ensuring everything is perfectly aligned and stable.
- Trauma Surgery: When a patient has complex facial or pelvic fractures, CT scans provide the essential blueprint surgeons need to reconstruct the anatomy just as it was.
- Neurosurgery: For any procedure involving the skull, like a craniotomy or placing deep brain stimulation electrodes, CT is simply invaluable.
Magnetic Resonance Imaging: Unlocking Soft Tissue Secrets
While CT is king for bone, Magnetic Resonance Imaging (MRI) is the master of seeing soft tissues. Instead of X-rays, an MRI uses powerful magnets and radio waves to generate breathtakingly detailed images of the brain, organs, muscles, and ligaments.
If a CT scan gives you the architectural blueprint of a building’s steel frame, an MRI reveals all the intricate wiring, plumbing, and interior finishes. This makes it absolutely essential for surgeries where steering clear of delicate soft tissue is the top priority.
The real power of an MRI is its incredible ability to tell different tissue types apart. A surgeon can see the exact border where a brain tumor ends and healthy tissue begins, or spot a tiny tear in a ligament that would be completely invisible on a CT scan.
MRI-guided surgery is a game-changer in:
- Neurosurgery: It has become the gold standard for brain tumor removal, helping surgeons get as much of the tumor as possible while carefully preserving critical brain function.
- Spinal Surgery: An MRI clearly illuminates the spinal cord and nerves, guiding a surgeon's hands as they decompress a pinched nerve without causing further injury.
- Prostate and Liver Surgery: It enables incredibly targeted biopsies and tumor treatments by giving a crystal-clear view of the diseased tissue.
Fluoroscopy and Ultrasound: Seeing the Action in Real-Time
Sometimes, a static map just won't cut it. Surgeons often need to see what's happening right now, and that’s where Fluoroscopy and Ultrasound step in.
Fluoroscopy is basically a live X-ray video. It provides a real-time feed that lets surgeons watch their instruments move through the body, see dye flowing through blood vessels, or check the alignment of bones as they set them. It's the go-to for many cardiovascular and orthopedic procedures.
Ultrasound, on the other hand, uses high-frequency sound waves to create live images without any radiation. It’s fantastic for looking at soft tissues and fluid, making it perfect for guiding needles during a biopsy, placing central lines into veins, or checking blood flow on the spot.
Together, these dynamic imaging tools give surgeons the instant visual feedback they need to navigate fast-paced, high-stakes procedures with confidence.
Of course. Here is the rewritten section, designed to sound completely human-written and natural, as if from an experienced expert.
How IGS Is Changing the Game in Medical Specialties
The real magic of imaging guided surgery isn't just in the technology itself, but in how it solves specific, high-stakes problems in different operating rooms. This isn't some abstract improvement; it’s a practical tool that gives surgeons a level of precision that was simply unimaginable a generation ago. Whether navigating the brain's delicate pathways or rebuilding a skeleton's framework, IGS is fundamentally improving patient outcomes.
By giving the surgeon a live, data-rich map of the patient's anatomy, the technology provides the confidence to operate in complex areas. Let’s look at a few examples of how this actually works on the ground.
Neurosurgery: A Clear Path Through the Brain
Think about what it takes to remove a deeply seated brain tumor. The surgeon walks a razor's edge: they have to get all of the cancerous tissue out to prevent it from coming back, but they also have to avoid damaging the healthy tissue that controls speech, movement, or memory. Being off by a single millimeter can change a person's life forever. This is exactly where IGS becomes a neurosurgeon's most trusted partner.
The Challenge: A tumor is growing dangerously close to the motor cortex—the part of the brain that orchestrates voluntary movement. The mission is to remove every last cancer cell without compromising the patient's ability to walk or use their hands.
The IGS Solution:
- Mapping Before the Mission: It all starts with a detailed MRI scan before the surgery. This isn't just any scan; it uses advanced techniques like functional MRI (fMRI) to pinpoint not only the tumor's size and location but also the critical neural highways around it.
- Building the GPS: This data is fed into the IGS system, which constructs an interactive 3D model of the patient’s brain. This model becomes the surgeon's personalized GPS for the procedure.
- Navigating in Real-Time: In the OR, the surgical instruments are fitted with tiny trackers. As the surgeon works, the screen shows the exact position of their tools on the 3D model, updating live. They can see precisely how close they are to the tumor's edge and, more importantly, to the vital motor cortex.
With this guidance, the surgeon can confidently and aggressively remove the tumor, knowing exactly where the safe boundaries are. It turns a high-wire act into a meticulously planned mission, dramatically increasing the odds of success while protecting what makes the patient who they are.
With imaging guided surgery, the neurosurgeon is no longer just relying on anatomical landmarks. They are navigating with a live, personalized map that highlights every critical structure, making the 'unseen' visible and the complex manageable.
Orthopedic Surgery: Perfecting Joint Replacements
In orthopedics, particularly for hip and knee replacements, success is all about alignment. We're talking millimeters and degrees. If an implant is placed even slightly off-kilter, it can lead to chronic pain, premature wear and tear, and eventually, another major surgery to fix it. Traditionally, getting this right has been a combination of a surgeon's experience, feel, and a set of mechanical guides.
The Challenge: A patient needs a total hip replacement. The goal is to set the new artificial socket and stem at the perfect angle and orientation for that person's unique body, ensuring the new hip feels natural and lasts for decades.
The IGS Solution:
- CT-Based Planning: A pre-operative CT scan is used to create a perfect 3D replica of the patient's pelvis and femur. The surgeon can then perform the entire surgery virtually on a computer, choosing the best implant size and mapping out its exact placement for flawless biomechanics.
- Intraoperative Guidance: During the actual surgery, trackers are placed on the patient’s pelvis and the surgical tools. The IGS system acts like a carpenter's level and protractor, giving the surgeon live feedback to ensure the implant components are being positioned exactly according to the plan.
- Verified Accuracy: The surgeon can make tiny adjustments with sub-millimeter accuracy, getting real-time confirmation that the final placement is a perfect match to the digital blueprint before a single stitch is placed.
Using imaging guided surgery this way helps ensure the new joint works just as it should from day one. This means patients often recover faster, the implants last longer, and people get back to living their lives with less pain.
ENT Surgery: Navigating the Labyrinth of the Sinuses
Ear, Nose, and Throat (ENT) surgeons work in some of the most cramped and complex real estate in the human body. Sinus surgery is a prime example. It involves navigating a maze of tiny passages that sit right next to the eyes and the base of the skull.
The Challenge: A patient with chronic sinusitis needs an operation to clear out blocked passages. The surgeon has to remove inflamed tissue and thin bone without accidentally straying into the optic nerve or the delicate barrier separating the sinuses from the brain.
The IGS Solution: It’s elegantly simple. The system uses a pre-operative CT scan to generate a detailed roadmap of the patient's unique sinus anatomy. In the operating room, the very tip of the surgeon’s instrument is tracked, its location shown as a dot on that map. This lets the surgeon see exactly where they are at all times, allowing them to confidently clear blockages while maintaining a safe distance from those critical no-go zones. It transforms a procedure once done with limited visibility into a precise, much safer intervention.
AI and Robotics: The Next Frontier in Surgery
Imaging guided surgery has been a massive leap forward, giving surgeons an incredible "map" to work with. But this is just the beginning. The next chapter is all about combining that map with artificial intelligence (AI) and robotics, moving surgery from simply being guided to becoming predictive, automated, and hyper-personalized.
Think of it this way: what if the map wasn't just a static 3D model, but a living, thinking guide? That's what AI brings to the table. By training algorithms on thousands of medical scans, AI learns to do things that would take a human expert precious time. It can instantly highlight the precise edges of a tumor, spot critical blood vessels buried in tissue, and even predict how that tissue might move or change once the procedure begins.
This turns the OR into a dynamic environment where the system doesn't just show the surgeon where to go—it warns them about potential problems before they even happen.
AI as the Surgeon's Co-Pilot
In the operating room of the near future, AI will act as an incredibly sharp co-pilot. Its ability to analyze visual information surpasses human limits, adding a powerful layer of insight that complements the surgeon's own skill and judgment. This isn't just about seeing better; it's about understanding what's being seen on a much deeper level.
This intelligent analysis brings some very real benefits to the operating table:
- Automated Segmentation: Instead of manually tracing organs or tumors on a CT scan, AI can do it instantly and with perfect accuracy. This saves time and makes sure nothing is missed.
- Predictive Modeling: Algorithms can run a quick simulation showing what might happen if an incision is made or a tumor is removed, helping the surgeon map out the safest and most effective path forward.
- Intraoperative Alerts: The system can sound a real-time alert if a surgical tool gets too close to a major nerve or artery that was identified on the pre-op scans.
We're already seeing this technology move from the lab into the clinic. Tools like the Clinic AI Assistant are demonstrating how AI can be applied today to support medical professionals in their daily workflow.
The goal of adding AI to imaging guided surgery isn't to replace the surgeon. It's about augmenting their skills—providing an intelligent safety net that reduces mental strain and frees them up to focus completely on the delicate work at hand.
Robotics: Bringing Superhuman Precision to the Scalpel
Robotics adds a whole new dimension to this evolution. A surgeon's hands, no matter how skilled and steady, are still human. They're subject to tiny, natural tremors and physical limitations. Robotic platforms, driven by the IGS system, can translate a surgeon's commands into movements with superhuman precision and steadiness.
When you pair a surgical robot with an AI-powered navigation system, you get something incredible. The robot can perform complex maneuvers in incredibly tight spaces with a level of accuracy that's nearly impossible to achieve by hand. This synergy between sight (IGS and AI) and action (robotics) is where we'll see the biggest advances in minimally invasive surgery. The robot's instruments, following the digital map flawlessly, can execute every movement without the slightest tremor.
This powerful combination of technologies is attracting serious investment. North America is currently at the forefront of the image-guided therapy market, holding a 42.1% share with revenues hitting around USD 2.2 billion. This lead is driven by the early adoption of advanced imaging and robotics from industry pioneers who are pushing the boundaries of what's possible when you combine real-time imaging with robotic precision. You can learn more about this growing market and its key players.
Augmented Reality: Blending the Digital and Physical Worlds
Perhaps the most exciting glimpse into the future comes from augmented reality (AR). Imagine a surgeon no longer having to look away from the patient to check a monitor. With AR, they can essentially "see through" the patient.
Using a special headset, the 3D anatomical model from the IGS is projected directly onto the surgeon's field of view, right on top of the patient. This seamlessly blends the digital guide with the physical reality of the operating room. The surgeon could see the exact location of a tumor or a critical blood vessel highlighted on the patient's body, providing a far more intuitive and direct form of guidance. This fusion of realities promises to make even the most complex procedures safer and more efficient.
Frequently Asked Questions About Imaging Guided Surgery
Hearing that you need surgery can be a lot to take in, and when new technologies are involved, it’s natural to have questions. Getting a handle on the tools and methods your surgical team will use is a huge step toward feeling prepared and confident. When it comes to imaging guided surgery, many patients and their families find themselves asking the same things.
We've put together some straightforward answers to the most common questions we hear. Our goal is to pull back the curtain on this technology and give you the clarity you need as you get ready for your procedure.
Is Imaging Guided Surgery Safe?
Yes, absolutely. In fact, making surgery safer is the whole reason this technology exists. By giving your surgeon a real-time, high-definition map of your body, it helps them steer clear of critical structures like major blood vessels, nerve bundles, and delicate brain tissue.
Think of it this way: it’s the difference between driving down a pitch-black country road and driving that same road with a state-of-the-art GPS and powerful headlights. The guidance system is there entirely to prevent missteps.
It's true that some imaging techniques, like CT scans or fluoroscopy, involve controlled doses of radiation. However, the immense benefit of that added accuracy—which leads directly to fewer complications, better results, and a smoother recovery—almost always outweighs the minimal exposure. Patient safety isn't just a feature; it's the core principle behind imaging guided surgery.
How Is IGS Different from Robotic Surgery?
That's a fantastic question. The two often get mentioned together and can even be used in the same operation, but they do two very different jobs. An analogy might help here.
Imagine you're building a highly intricate piece of custom furniture. Imaging guided surgery is the detailed digital blueprint and the laser level you're using to make sure every single cut and connection is perfect. Robotic surgery, on the other hand, is the set of incredibly precise power tools that carries out the physical work based on that blueprint.
To put it simply:
- Imaging Guided Surgery (IGS) is the navigation system. It’s the brain of the operation, creating the map and tracking the surgeon’s instruments in real-time. Its job is to provide information and guidance.
- Robotic Surgery is the execution system. It’s the hands of the operation. The surgeon controls highly advanced mechanical arms that perform the physical movements, eliminating natural hand tremors and allowing for incredible dexterity in tight spaces.
Many of the most advanced procedures today combine the two. The IGS "brain" provides the live map that guides the robotic "hands," achieving a level of precision that was once thought impossible.
What Are the Main Benefits for Patients?
This is really the most important question—how does all this technology actually help you? The advantages are significant and touch on nearly every aspect of the surgical experience, from the moment you enter the OR to your recovery back home.
Here are the key benefits patients see:
- Smaller Incisions: Surgeons can navigate with such pinpoint accuracy that they don't need large openings to see what they're doing. This means less trauma to the surrounding skin and muscle.
- Less Pain and Blood Loss: It's a simple equation: smaller, more precise work leads to less post-op pain and minimal blood loss.
- Shorter Hospital Stays: Because the procedure is less invasive, the body has less healing to do. Patients who have procedures with imaging guided surgery often get to go home much sooner.
- Better Surgical Outcomes: This level of accuracy dramatically increases the chances of a successful surgery, whether that means removing every last bit of a tumor or positioning a new joint implant perfectly for decades of comfortable use.
All these factors add up to a surgical process that is not only safer but also has a much gentler impact on your body, helping you get back to your normal life faster.
Is This Technology Available Everywhere?
While IGS is quickly becoming the gold standard for many complex operations in fields like neurosurgery and orthopedics, it hasn't made its way into every single hospital just yet. These systems represent a major investment in both equipment and specialized team training.
You're most likely to find IGS technology in:
- Major academic medical centers
- University-affiliated teaching hospitals
- Specialized surgical institutes
The good news is that as the technology matures and becomes more accessible, its footprint is constantly expanding. It's moving into a much wider range of hospitals, making this higher standard of care available to more people every year. If you're looking at a surgical procedure, don't hesitate to ask your surgeon if they use imaging guided surgery.
At PYCAD, we're on the front lines of blending AI with medical imaging to build smarter, more intuitive surgical platforms. We specialize in the data management, model training, and deployment that medical device companies need to engineer the next generation of tools for the OR—solutions that boost diagnostic certainty and make surgery more efficient. See how our AI services are shaping the future of medical technology.