The DICOM standard isn't just another file type; it's the universal translator for the world of medical imaging. It's the reason a CT scan from a scanner in one country can be opened, read, and analyzed on a radiologist's workstation halfway across the world. Without it, we'd be stuck in a digital version of the Tower of Babel, with every machine speaking its own unique, incompatible language.
The Foundation of Modern Medical Imaging
Think about what would happen if every brand of medical scanner—from GE to Siemens to Philips—saved images in its own proprietary format. A surgeon's software wouldn't be able to open an MRI from the hospital across town. This is the chaos that DICOM was designed to prevent.
DICOM, which stands for Digital Imaging and Communications in Medicine, is far more than a simple format like JPEG or PNG. It’s a comprehensive set of rules governing how medical images are created, stored, and shared. This shared language ensures that an X-ray taken in a small rural clinic can be perfectly interpreted by advanced software in a major urban hospital, making true collaboration in patient care possible.
More Than Just Pixels
What truly sets DICOM apart is how it bundles crucial patient information directly into the image file itself. This isn't just a picture; it's a complete, self-contained medical record. This attached data, or metadata, provides the context a doctor needs to make an accurate diagnosis.
Without that context, a medical image is just a collection of pixels. With it, the image tells a full story. This data typically includes:
- Patient Demographics: Name, date of birth, and patient ID to ensure you're looking at the right person.
- Acquisition Details: What machine was used (e.g., MRI, CT), the specific settings, and the exact date and time of the scan.
- Positional Information: Key details about the patient’s orientation and which part of the body was scanned.
By packaging the image and its data into a single object, DICOM eliminates the dangerous risk of mixing up patient files and gives clinicians everything they need in one place.
A Standard Born from Collaboration
As medical imaging went digital, the need for a common standard became glaringly obvious. The first versions were developed in the 1980s, but it was the third iteration, released in the early 1990s by the American College of Radiology (ACR) and the National Electrical Manufacturers Association (NEMA), that became the DICOM we know today.
Its name was officially changed to reflect its broader scope, moving beyond just radiology to embrace disciplines like cardiology, pathology, and dentistry. If you're curious about the specifics, you can explore its history to see how it evolved into the international benchmark for medical imaging.
By establishing a common ground for all imaging modalities, DICOM removes technical barriers, allowing doctors to focus on what truly matters: accurate diagnosis and effective patient treatment.
The Building Blocks of DICOM
To really get a handle on how DICOM works its magic, you need to understand its three core components. Think of them as a system, much like a specialized courier service, designed to package, label, and securely transport medical images and their data across a complex healthcare network.
Each part has a very specific job. One defines what the package (the file) looks like, another dictates the commands used to move it, and the last is the rulebook that ensures every device speaks the same language. Let's break them down.
The DICOM File Format: The Smart Data Package
A DICOM file isn't just a picture. It’s a world away from a simple JPEG or PNG. A better way to think of it is as a highly intelligent, self-contained data package. Inside this digital container, you don't just find the image itself; you also get a comprehensive set of metadata that is permanently attached to it.
This metadata is the file's brain. It contains all the contextual information needed for a proper diagnosis and for maintaining accurate records. It’s all right there, locked together. This includes details like:
- Patient Information: The patient's full name, ID number, and date of birth to ensure the image is always tied to the right person.
- Acquisition Context: The nitty-gritty details about the scan itself—what machine was used (CT, MRI, etc.), the exact technical settings, and when it happened.
- Anatomical Details: Crucial information about the body part scanned and how the patient was positioned.
This all-in-one structure is a core principle of DICOM. It guarantees that the clinical context never gets separated from the pixels, which is absolutely critical in a medical setting.
DICOM Network Services: The Language of Action
So, if the DICOM file is the package, the DICOM Network Services are the action words—the commands that tell other devices on the network what to do with that package. Officially, these are called DICOM Message Service Elements (DIMSEs), and they are the foundation for communication.
Think of DIMSEs as the set of universal verbs that every DICOM-compliant machine understands. They are the standardized instructions for sending, finding, and pulling medical imaging data, making sure every system, regardless of the manufacturer, speaks the same operational language.
These commands are what drive a real-world clinical workflow. For example, after a scan is complete, the CT scanner uses a C-STORE command to send and store the new study on the hospital’s central PACS (Picture Archiving and Communication System). A little while later, a radiologist at their workstation uses a C-FIND command to search for that patient's study and a C-MOVE command to retrieve it for review.
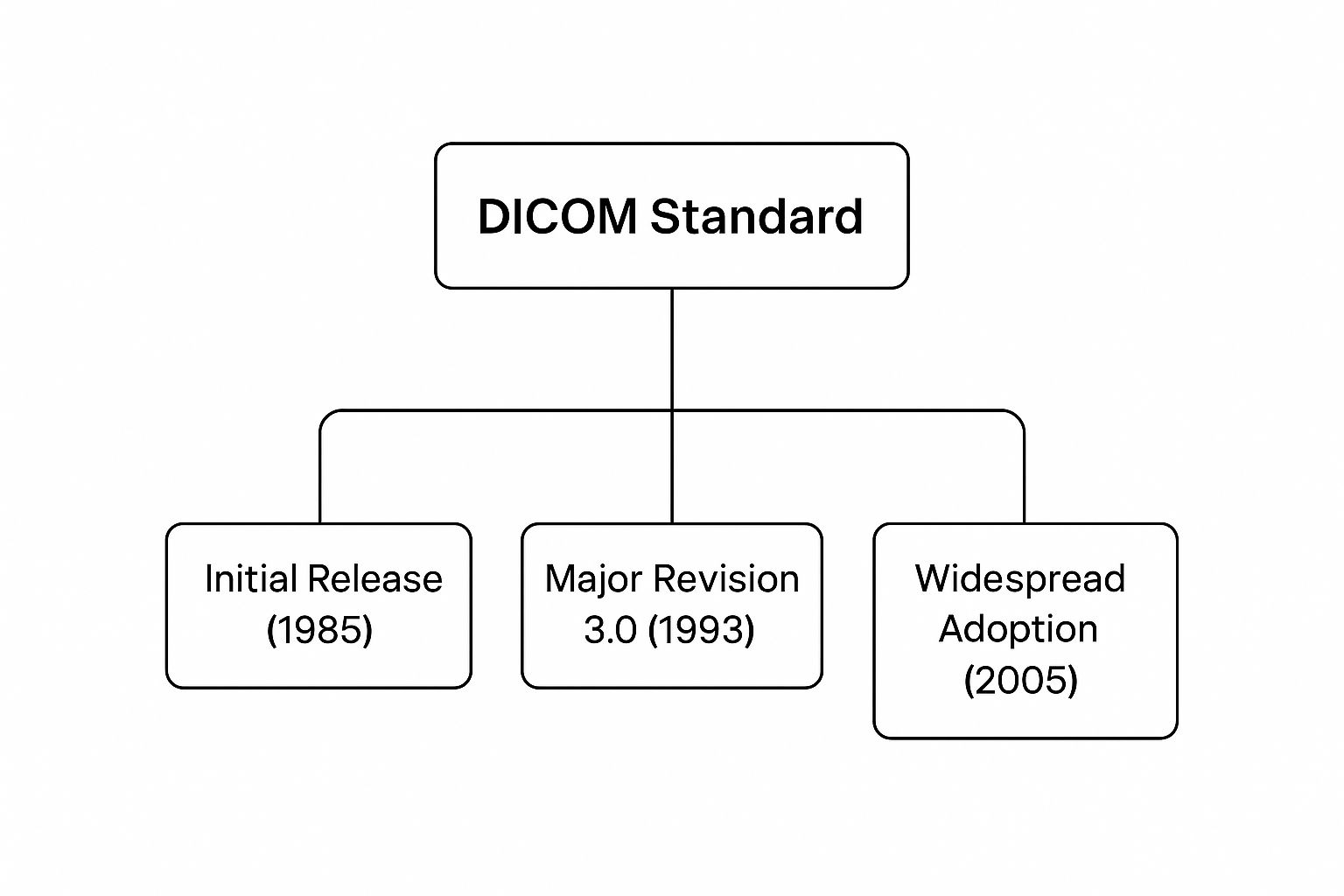
This evolution is key. The major revision in 1993 was the real game-changer, setting the stage for DICOM to become the industry-wide standard it is today.
DICOM Conformance Statements: The Interoperability Rulebook
The final piece of this puzzle is the DICOM Conformance Statement. This is a technical document—basically an instruction manual—that every manufacturer must publish for its products. It spells out exactly which DICOM services and file types the device can handle.
It's a bit like checking the specs before you buy two different brands of walkie-talkies to make sure they can communicate on the same frequency. The Conformance Statement does the same thing, but for multi-million dollar medical equipment. It lets a hospital’s IT team confirm that a new MRI scanner can actually "talk" to their existing PACS before they sign the purchase order.
Carefully reviewing these statements is how you prevent interoperability nightmares. It's the step that ensures all the different pieces of a hospital's imaging ecosystem can work together as one cohesive unit. Without them, seamless, vendor-neutral communication would just be a pipe dream.
How DICOM Powers a Real Clinical Workflow
The theory behind the DICOM standards is one thing, but watching it work in a real hospital setting shows you its true genius. To bring these concepts to life, let’s follow a patient’s journey and see how this invisible network of data exchange supports every critical decision.
Imagine a patient—we'll call her Jane—arrives at the emergency room after a bad fall. The ER doctor suspects an internal injury and immediately orders an urgent CT scan of her abdomen. That single order sets off a sophisticated chain reaction, all quietly managed by DICOM.
From Scan to Storage: The First Connection
Down in the imaging suite, the CT scanner gets to work, capturing hundreds of detailed images. Once the scan is finished, the machine doesn't just dump a folder of JPEGs onto a server. Instead, it creates a series of DICOM objects. Each image file is instantly embedded with Jane's patient ID, the scan date, and specific technical details from the scanner itself.
Next, the CT scanner uses a DICOM network service called C-STORE to push these newly minted image objects across the hospital network. Their destination? The heart of the imaging department: the Picture Archiving and Communication System (PACS). Think of the PACS as a vast, hyper-organized digital library that receives the data and instantly files it under Jane’s electronic record.
This initial transfer is the first crucial link. The C-STORE command ensures the high-fidelity images and their vital metadata travel together from the scanner to central storage, virtually eliminating the risk of data loss or patient mix-ups.
This entire process hums along in the background, often taking just a few minutes. It's a perfect illustration of how DICOM enables complex machine-to-machine communication without a person having to lift a finger, making sure the right data gets to the right place, fast.
Retrieval and Diagnosis: The Radiologist's Workflow
Now, a radiologist in a different building needs to read the scan. From their high-resolution diagnostic workstation, they don’t need to hunt through confusing server folders. Their software sends a C-FIND command to the PACS, essentially asking, "Show me all recent studies for this patient."
The PACS instantly replies with a list of matching scans. The radiologist selects the correct one, and their workstation then sends a C-MOVE command. This instructs the PACS to send the complete set of CT images over to the radiologist's machine. This "pull-on-demand" approach is incredibly efficient, moving large files only when they are actively needed.
The radiologist can now dive into the images, measure structures, and form a diagnosis. Their expert findings, along with any annotations, can be saved as another DICOM object—typically a Structured Report—and sent right back to the PACS, where it's permanently linked to the original study.
Collaboration and Treatment Planning: The Final Step
Finally, the surgeon who will handle Jane’s procedure needs to see everything. Using their own software, they can also query the PACS and retrieve the entire study, complete with the radiologist's detailed notes. This seamless flow means every single person on Jane’s care team is working from the exact same complete, up-to-the-minute information.
This kind of interoperability is the norm today because DICOM standards have achieved massive global adoption since their creation. What started in radiology with CT and MRI has since expanded to cardiology, ophthalmology, digital pathology, and even dentistry. Today, virtually every medical imaging device and software platform from major manufacturers is built to be DICOM-compliant, making workflows like Jane's not just possible, but routine. This widespread collaboration is the ultimate payoff of the standard, directly improving patient outcomes by enabling faster, better-informed decisions.
Getting DICOM Implementation and Security Right
While the DICOM standard gives us a solid blueprint for medical imaging, making it work in the real world is another story entirely. It demands careful planning and a keen eye for detail. You can't just buy DICOM-compliant equipment and expect it to work flawlessly out of the box. Think of it less like flipping a switch and more like assembling a complex puzzle—every single piece needs to fit perfectly with the others.
One of the most critical steps, and one that's surprisingly easy to overlook, is to thoroughly review the DICOM Conformance Statements before you buy anything. These technical documents are the instruction manuals that spell out exactly what a device can and cannot do. Skipping this review is a massive gamble that can lead to expensive headaches, like a new scanner that can send an image (C-STORE) but can't answer search queries (C-FIND) from your main PACS.
Doing this homework upfront prevents these kinds of interoperability gaps. It’s what separates a smooth, connected workflow from a frustrating cycle of troubleshooting and data silos.
You Have to Build Security In
In healthcare, exchanging data and securing it are two sides of the same coin. Protecting patient information isn't just a good idea; it's a legal and ethical obligation. The DICOM standard itself isn't inherently insecure, but its implementation requires you to actively add security measures to keep data safe from prying eyes.
The most basic layer of defense is encryption. By using DICOM-TLS (Transport Layer Security), you can encrypt imaging data as it travels between devices, like from a CT scanner to a PACS server. This creates a secure, private tunnel that makes the data unreadable to anyone trying to intercept it on the network. In any modern setup, this should be considered the absolute baseline, no exceptions.
"A common misconception is that DICOM is 'secure by default.' In reality, security is an active process. It relies on IT teams implementing available tools like encryption and access controls to build a fortress around patient data, not just a fence."
Beyond just protecting data in transit, a strong security posture involves several other layers:
- Strict Access Controls: Put role-based access controls in place so that clinicians and staff can only see or change the data they need for their jobs. A radiologist needs full access, but someone in billing might only need to see the metadata.
- Data-at-Rest Encryption: The hard drives on your PACS servers and archives must be encrypted. This way, even if the physical hardware is stolen, the patient data remains protected.
- Regular Security Audits: Keep a close eye on network logs and run regular audits. This helps you spot and react to suspicious activity before it turns into a major breach.
Avoiding Common Implementation Pitfalls
Even with the best-laid plans, a few common problems can trip you up during a DICOM implementation. A major one is inconsistent metadata handling between different vendors. Sometimes called "tag morphing," this is what happens when two systems fill out the same DICOM tag in slightly different ways. It can lead to corrupted patient records or break automated workflows.
Data migration is another huge challenge. Moving years or even decades of imaging studies from an old PACS to a new one is a monumental task. You run the risk of incomplete transfers, data corruption, and major headaches trying to reconcile different vendor formats. Trying to get older, non-compliant equipment to play nice is also a tough nut to crack, often requiring expensive gateway systems to translate data into the proper DICOM format.
A solid implementation and security strategy is absolutely essential. To put it in perspective, a 2016 global security scan found a shocking 2,774 unprotected DICOM servers worldwide, with hundreds of them completely open to the public internet. This research highlights a critical point: the standard provides the tools for security, but without proper implementation, huge amounts of sensitive patient data are left vulnerable. You can learn more about these security issues in the full study on radiology data infrastructure.
DICOM Implementation Best Practices
To make things a bit easier, here’s a quick-reference guide on what to do—and what to avoid—when deploying and managing your DICOM systems.
| Do | Don't |
|---|---|
| Thoroughly vet Conformance Statements before purchasing new equipment. | Assume "DICOM compliant" means full interoperability with your existing systems. |
| Enable DICOM-TLS encryption for all data transmitted over the network. | Leave data unencrypted, exposing it to interception and breaches. |
| Implement strict role-based access controls to limit data access to only those who need it. | Give everyone broad access, increasing the risk of insider threats or errors. |
| Plan data migrations meticulously with extensive testing and validation. | Rush a migration without a rollback plan, risking data loss or corruption. |
| Conduct regular security audits and monitor network logs for suspicious activity. | Set it and forget it. Security is an ongoing process, not a one-time task. |
Following these best practices isn’t just about technical correctness; it’s about building a reliable and secure imaging infrastructure that clinicians can trust and that keeps patient data safe.
DICOM's Crucial Role in Medical AI

The relationship between Artificial Intelligence and the DICOM standard is more than just a convenience; it's a foundational partnership. AI in medicine hinges on training algorithms with enormous amounts of high-quality, perfectly structured data. In this world, DICOM is the essential framework that makes it all work.
Think of an AI model as a brilliant student who needs to learn from a massive library. If every book in that library were written in a different language with its own unique structure, the student would get nowhere fast. DICOM is the universal translator and grammar guide, ensuring every "book"—each medical image and its related data—is presented in a consistent, machine-readable format.
The real magic for AI lies in the rich metadata embedded in every DICOM file. This isn't just about the pixels that make up the image. It’s about the context—patient demographics, scanner settings, acquisition details—that allows an AI to discover subtle patterns humans might never see. This consistency is what lets developers build robust and genuinely accurate diagnostic tools.
Structuring AI's Output for Clinical Use
An AI's job isn't done once it flags an anomaly. For an algorithm’s findings to be truly useful in a clinical setting, they have to fit seamlessly back into the existing workflow. This is where a specific part of the DICOM standard, DICOM-SR (Structured Reporting), becomes incredibly important.
DICOM-SR provides a standardized template for communicating what the AI found. It allows outputs—like precise tumor measurements, risk classifications, or heatmaps—to be saved and shared in a structured, searchable format. An AI's output becomes more than just a static note; it's a dynamic piece of data that can be filed, queried, and analyzed just like any other part of the patient's record. This integration is what connects the high-tech world of AI with the practical reality of daily patient care.
The true power of medical AI is unlocked when its insights can be smoothly integrated into a radiologist's workflow. DICOM-SR provides the bridge, transforming an algorithm’s output from a simple suggestion into a quantifiable, actionable piece of the diagnostic puzzle.
As AI's dependence on DICOM grows, understanding how to build these applications is key. Exploring resources on development, including those that detail no-code backend AI solutions, can offer a practical look at implementation.
Evolving to Support New Forms of AI Data
The DICOM standard is anything but a static document. It's a living framework that constantly evolves to keep pace with technology. As medical imaging AI has become more sophisticated, the standard has adapted to handle entirely new kinds of data generated by these advanced algorithms.
For instance, modern AI models produce outputs that are far more complex than simple numbers or text. These can include:
- Segmentation Maps: Overlays that precisely outline anatomical structures or abnormalities, like painting the exact borders of a tumor on a CT scan.
- Probability Heatmaps: Visual guides that show the likelihood of a condition across an image, directing a clinician's attention to high-risk areas.
- Attention Maps: These fascinating visuals show which parts of an image the AI "focused" on to reach its conclusion, offering a peek into its decision-making process.
The DICOM committee is always working to create new Information Object Definitions (IODs) to formally support these AI-specific data types. By standardizing how this information is stored and sent, DICOM guarantees that these powerful insights can be shared and viewed across different systems, regardless of the vendor. This constant evolution shows DICOM isn't a legacy protocol but a forward-thinking framework actively shaping the future of AI in medicine.
The Future of DICOM: Moving to the Web and Cloud
For decades, the DICOM standard was the backbone of medical imaging within the four walls of a hospital. It was designed for the secure, private networks connecting scanners to workstations. But healthcare doesn't live solely on-premise anymore. With the rise of teleradiology, mobile access, and AI-driven diagnostics, imaging needs to be accessible anywhere, anytime. This is where the next evolution of DICOM comes in: DICOMweb.
Think of it like this. Traditional DICOM is a bit like a closed-circuit television system—incredibly reliable and secure, but built for a specific location. DICOMweb is the upgrade to a secure, global streaming service. It takes the core principles of DICOM and re-imagines them for the internet, using the same web technologies that power our daily lives.
From Old-School Protocols to Modern APIs
At its heart, DICOMweb swaps out the old, specialized network protocols for a set of modern, web-friendly ones. These new standards are built on RESTful APIs, the same architecture that developers use to build today's mobile and web apps. This is a game-changer because it means developers no longer need deep, esoteric knowledge of legacy DICOM networking to work with medical images.
These web-native protocols cover the same ground as their predecessors, just in a much more intuitive way:
- STOW-RS (Store Over the Web): This is the new C-STORE. It's how a modern application, like a mobile app or web portal, can securely send and save medical images to a cloud archive.
- QIDO-RS (Query based on ID for DICOM Objects): The replacement for C-FIND. It lets you search for patient studies or images with simple web queries—much like finding a product on an e-commerce site.
- WADO-RS (Web Access to DICOM Objects – RESTful): This protocol takes over from C-MOVE, handling how you retrieve images. It’s incredibly flexible, letting an app grab an entire study, one specific image, or even just the metadata.
Thanks to this shift, a radiologist can now pull up a patient's CT scan on a tablet from home, review the images securely in a web browser, and never have to install a single piece of proprietary software.
DICOMweb is the essential bridge connecting the isolated world of on-premise medical imaging with the vast potential of the cloud. By speaking the language of the web—HTTPS and RESTful APIs—it opens the door to incredible scalability, accessibility, and new possibilities for patient care.
Unlocking the Power of Cloud-Based Imaging
This move to web-based communication is precisely what allows healthcare organizations to fully embrace cloud computing for their imaging needs. With DICOMweb, a hospital's massive Picture Archiving and Communication System (PACS) or Vendor Neutral Archive (VNA) can finally break free from the on-site server room and live in the cloud.
The benefits are immediate and substantial. First, you get nearly infinite scalability. Hospitals are no longer stuck in a cycle of buying, managing, and replacing expensive physical servers to keep up with the explosive growth of imaging data. The cloud scales on demand, which is a much more efficient and cost-effective model.
Second, it provides a level of disaster recovery that most on-premise setups can't match. If a hospital's local infrastructure is hit by a flood, power outage, or cyberattack, having a secure, replicated copy of all patient imaging data in the cloud ensures that it remains safe and accessible. This shift also dramatically simplifies data sharing for things like multi-center clinical trials and makes teleradiology workflows smoother than ever.
DICOMweb isn't just a technical tweak. It's a fundamental enabler for a more connected, resilient, and intelligent future for medical imaging.
Frequently Asked Questions About DICOM
When you're dealing with medical imaging, a lot of technical questions come up. To help cut through the noise, here are some straightforward answers to the questions we hear most often about the DICOM standards.
Is DICOM Just for Radiology?
Not at all. While DICOM got its start in radiology—think CT scanners and MRIs—it’s grown far beyond its original home. Today, it’s the universal language for just about any medical discipline that generates images.
You’ll find it used in:
- Cardiology: For echocardiograms and angiograms.
- Pathology: With whole-slide digital images of tissue samples.
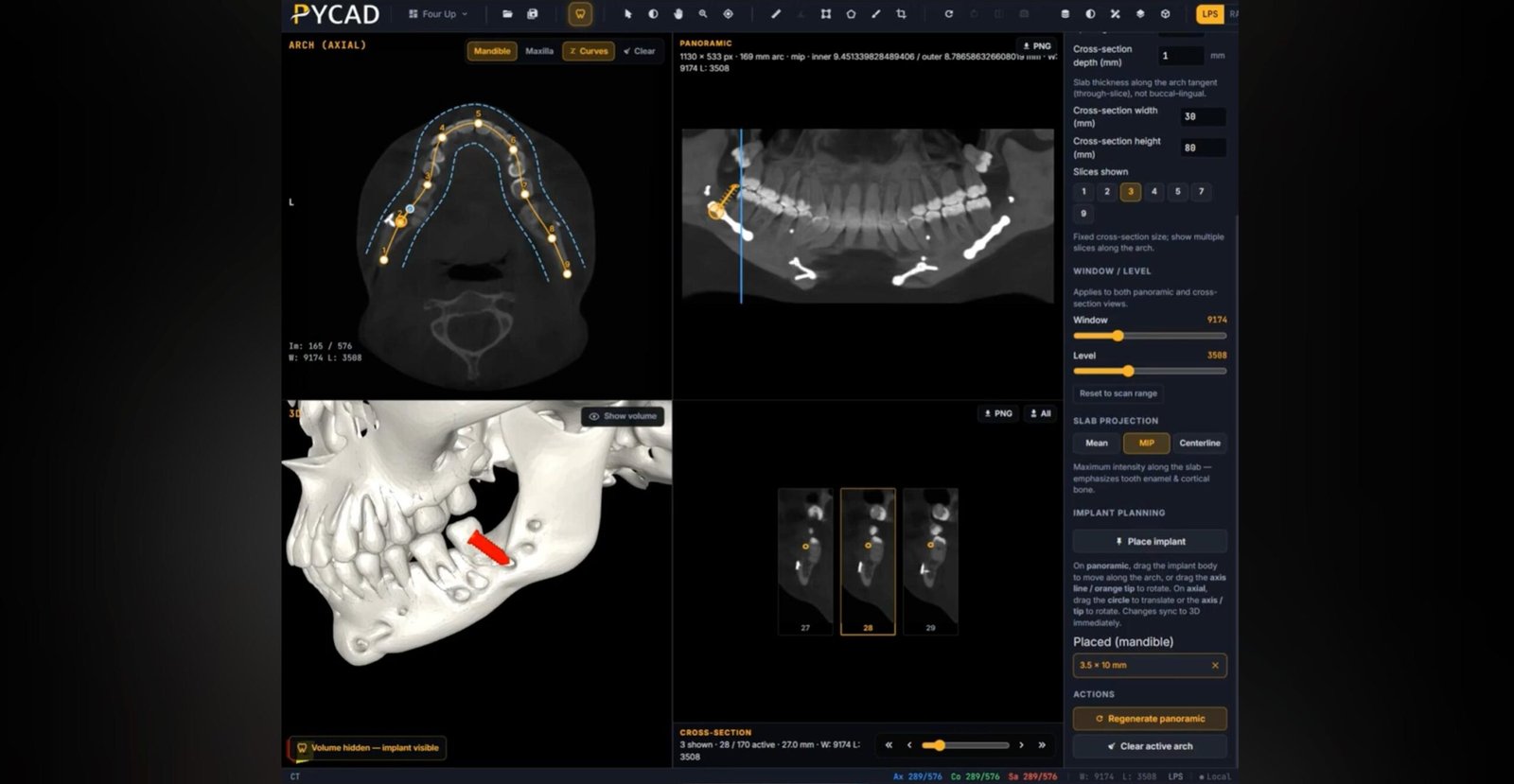
- Dentistry: Handling digital X-rays and 3D scans.
- Ophthalmology: For retinal scans and other diagnostic pictures.
The bottom line is, if a piece of medical equipment creates an image, you can bet it uses DICOM to make sure that image can be properly stored, shared, and viewed.
What Is the Difference Between DICOM and HL7?
This is a classic point of confusion, but it’s easy to clear up with an analogy. Think of DICOM and HL7 (Health Level Seven) as two different specialists in a hospital who have to coordinate patient care. They both manage crucial information, but they handle very different types of it.
DICOM is the imaging specialist. Its entire structure is built to handle the big, complex image files and all the metadata that goes with them. HL7 is the administrative and clinical data specialist. It focuses on text-based information, like patient admissions, billing details, and lab results.
Here’s how they work together: An order for a CT scan is placed in the hospital's main system, which sends an HL7 message to the radiology department to schedule it. After the scan is done, DICOM takes over, sending the actual images to the PACS for a radiologist to review. They are two distinct but essential standards that frequently pass the baton to each other.
Can I View a DICOM File on Any Computer?
No, at least not without the right software. A DICOM file isn't like a regular JPEG or PNG that you can just double-click to open. It’s a complex container holding not just the image but a wealth of protected medical information, so you need a dedicated DICOM viewer.
These specialized viewers are built to correctly read the file’s structure, display the image with the necessary clinical fidelity, and give clinicians tools for analysis, like making measurements or adjusting contrast. Plenty of excellent free and commercial viewers are out there, but you can't just open a .dcm file in your computer’s default photo app and expect it to work.
At PYCAD, we specialize in putting DICOM data to work, building and deploying sophisticated AI solutions for medical imaging. From anonymizing data to deploying production-ready models, we partner with medical device companies to boost diagnostic accuracy and streamline operations. Learn how we can support your next project by visiting us at https://pycad.co.