Think of DICOM as the universal language for medical imaging. It’s the reason a radiologist in New York can flawlessly open and analyze a CT scan taken in Tokyo. This standard is the bedrock of digital medicine, defining not just the file format for an image, but also the network rules for sharing it.
Why DICOM Standards Are the Bedrock of Modern Healthcare
Can you imagine a world where every medical scanner—from MRI machines to ultrasound wands—spoke a different digital dialect? A specialist at one hospital wouldn't be able to open an X-ray from another clinic. This was the chaotic reality of early medical imaging, a "digital Tower of Babel" that created dangerous delays and information silos.
DICOM (Digital Imaging and Communications in Medicine) was created to solve this exact problem. It serves as a universal translator, establishing a single, globally understood framework for medical images and all the critical information attached to them. Thanks to DICOM, a CT scan, an MRI, or a digital pathology slide isn't just a picture; it's a complete, portable medical record.
The Problem DICOM Solved
Before DICOM, healthcare providers were often trapped in proprietary ecosystems. If a hospital bought a scanner from one company, they were usually forced to buy the viewing stations and storage systems from that same company just to make sure everything worked together. This stifled innovation, drove up costs, and made sharing vital patient data between different doctors a logistical nightmare.
The DICOM standard broke down those digital walls. It created a common ground, allowing devices from competing manufacturers to finally speak the same language. First published in 1985 through a joint effort by the American College of Radiology (ACR) and the National Electrical Manufacturers Association (NEMA), it completely reshaped the field. Today, it’s estimated that over 90% of major hospitals worldwide use DICOM-compliant equipment, a clear sign of its incredible success.
Key Insight: DICOM is far more than just a file format. It's a comprehensive ecosystem that governs how images are stored, queried, retrieved, and presented. This ensures consistency and reliability from the scanner to the specialist's screen.
This standardization underpins the entire modern medical imaging enterprise. It directly impacts diagnostic speed, clinical accuracy, hospital efficiency, and, most importantly, patient outcomes. Of course, the power of any standard is tied to how well it's documented, a principle that applies far beyond just DICOM. You can explore more on the importance of documentation standards to see how this concept plays out across industries.
Who Relies on DICOM Standards and Why
The standard's impact is felt across the entire healthcare landscape. From the doctors on the front lines to the engineers developing the next generation of medical AI, everyone has a stake in it.
The table below highlights the key players in the medical imaging world and why DICOM is so crucial for their work.
| Stakeholder | Primary Benefit |
|---|---|
| Radiologists & Clinicians | Guarantees access to high-fidelity images and patient data for accurate diagnosis, regardless of where the scan was performed. |
| Hospital IT Departments | Simplifies system integration and data management, reducing vendor lock-in and supporting interoperability across the enterprise. |
| Medical Device Manufacturers | Provides a clear, universal specification to build compliant hardware and software, ensuring market compatibility. |
| Medical AI Companies | Offers a structured data source with rich metadata, essential for training, validating, and deploying diagnostic algorithms. |
| Patients | Enables portability of their medical imaging records, facilitating second opinions and continuity of care between different providers. |
Ultimately, this web of reliance demonstrates just how deeply DICOM is woven into the fabric of patient care. It’s the invisible infrastructure that makes modern, collaborative medicine possible.
Understanding the Three Pillars of DICOM
To really get a handle on DICOM, you have to understand its three core components. I like to think of them as the three pillars holding up the entire world of medical imaging. They’re the reason a CT scan taken in one hospital can be read by a specialist in another, even if they use completely different equipment.
Think of it as a sophisticated logistics system designed specifically for medical images. You have the package itself, the delivery network, and a detailed instruction manual for every piece of equipment involved. Each pillar has a specific job, and together, they form the backbone of modern radiology.
Pillar 1: The DICOM File Format
First up is the DICOM file format. This is the standard for the .dcm files you see in medical imaging. It's so much more than just a picture. A normal image file, like a JPEG, just contains pixel data—the visual information. But a DICOM file is a complete, self-contained medical record.
A good analogy is a sealed digital envelope. Inside that envelope, you’ll always find two things:
- The Image: This is the raw, high-fidelity pixel data straight from the scanner (like an MRI or CT machine). It’s preserved with lossless quality, which is critical for accurate diagnosis.
- The "Letter": This is a huge bundle of metadata known as the DICOM header. It contains dozens of essential details like the patient’s name and ID, the exact date and time of the scan, the modality used, and even the specific settings on the machine that took the image.
This tight coupling of image and data is what makes a DICOM file so powerful. You can't separate the picture from its context.
The image below gives you a simple visual breakdown of how a DICOM file organizes all this information.
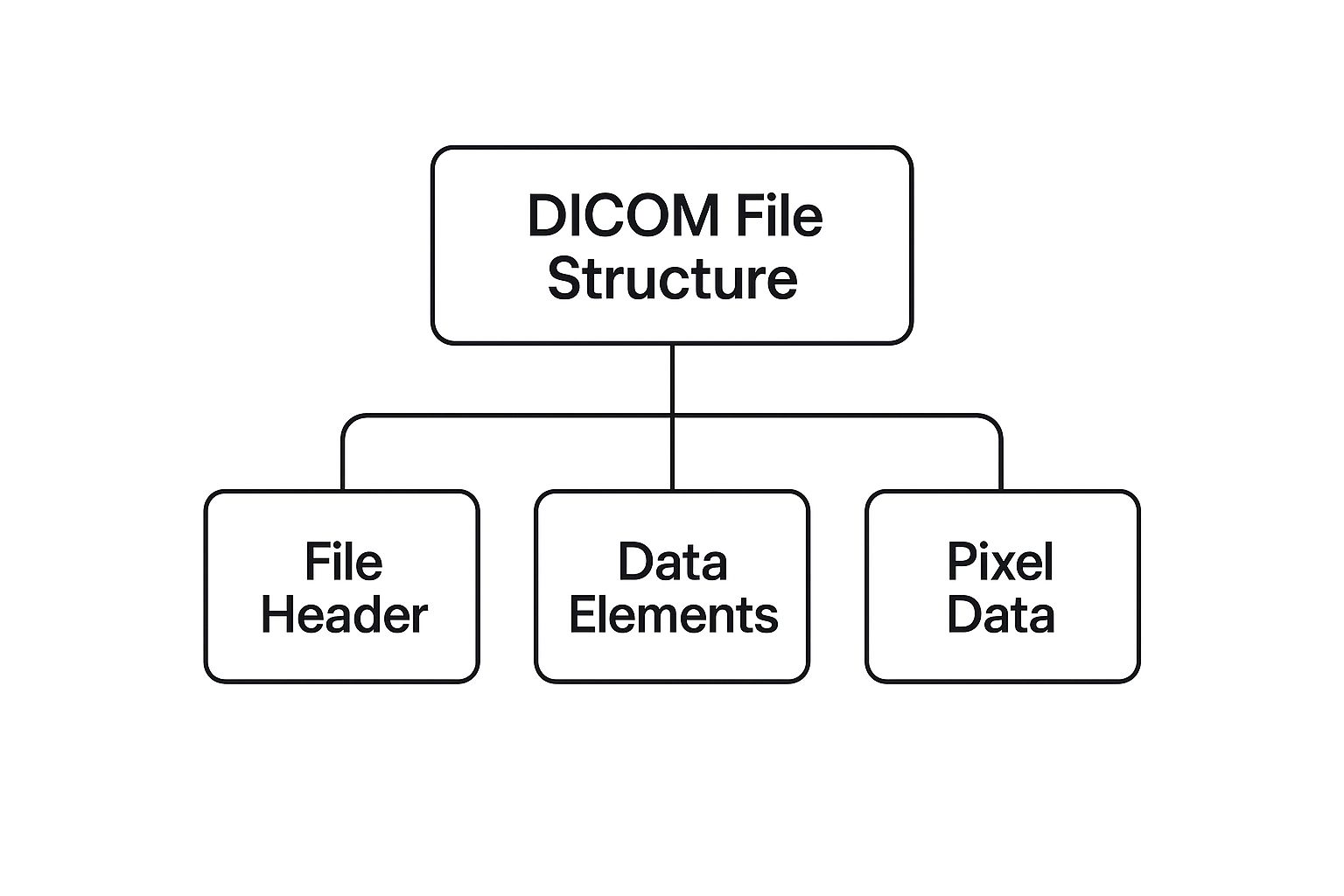
This structure guarantees that a clinician always has the full story, ensuring the image is a verifiable and complete record for diagnosis.
Pillar 2: DICOM Network Services
The second pillar covers DICOM Network Services. If the file format is the "package," then these services are the "postal system" that moves the packages around. This is the protocol that lets a scanner talk to a server, or a workstation pull images for a radiologist to review.
Formally, these services are called DICOM Message Service Elements (DIMSE). The names can sound a bit technical, but they map to very simple, real-world actions.
- C-STORE: This is the most basic and common service. It’s essentially a "send" or "save" command. A CT scanner uses C-STORE to push a newly acquired study to the hospital's Picture Archiving and Communication System (PACS).
- C-FIND: Think of this as a "search" function. A radiologist's workstation uses C-FIND to ask the PACS, "Do you have any studies for patient John Smith?"
- C-MOVE / C-GET: These are the "retrieve" commands. Once you've found the studies you need with C-FIND, you use C-MOVE or C-GET to pull the actual image files from the PACS to your local machine for viewing.
Because these commands are standardized, a Siemens scanner, a GE PACS, and a Philips workstation can all speak the same language. This is what creates a truly interoperable network.
Here's how it works in practice: A radiologist needs to compare a new chest X-ray with a patient's scans from last year. Their viewing software sends a C-FIND request to the hospital's PACS. The PACS replies with a list of matching studies. The radiologist clicks on the prior exam, and the software issues a C-MOVE request to download those images to their screen.
Pillar 3: The DICOM Conformance Statement
The third and final pillar is the DICOM Conformance Statement. This is a critical—and often overlooked—document. It’s basically a technical resume for any piece of medical equipment or software, detailing exactly what it can and can't do in the DICOM world.
Every single DICOM-compliant device has one. This document spells out, in no uncertain terms:
- Which DICOM services it supports (e.g., can it send with C-STORE? Can it search with C-FIND?).
- The roles it can play (Is it a sender, a receiver, or both?).
- The specific data formats and syntaxes it understands.
Before a hospital connects a new MRI machine to its network, the IT team and clinical engineers will sit down and compare the Conformance Statements of the new machine and their existing PACS. This lets them confirm compatibility before plugging anything in, preventing countless headaches and ensuring that everything will work together seamlessly from day one. It's the key to making "plug-and-play" a reality in a complex, multi-vendor environment.
How DICOM Evolved for the Web and Cloud

The DICOM standard was never meant to be a static document, gathering dust on a shelf. It has always evolved to keep pace with the real-world demands of medicine. Its original network protocols were brilliant for the closed, private networks inside a hospital, but the world changed. With the rise of the internet, cloud computing, and telehealth, DICOM needed to learn to speak a new language: the language of the web.
This need gave birth to DICOMweb, a modern, web-native extension to the core standard. It’s a collection of RESTful services that lets medical imaging data be accessed, shared, and managed using the very same web technologies that power the apps and websites we use every day.
Here's a simple analogy: think of traditional DICOM networking as a highly specialized, internal phone system for a single office building. It works perfectly within those four walls. DICOMweb, on the other hand, is like giving that system the ability to make secure calls over the global internet using standard smartphone technology. This shift has been absolutely critical for pushing medical imaging beyond the hospital walls.
The Rise of Web-Friendly DICOM Services
At its heart, DICOMweb offers a trio of services that mirrors the classic DICOM network functions but communicates using web-native protocols like HTTP/HTTPS. This is a game-changer because it makes it incredibly easy for developers to build applications that can talk to imaging archives without needing to master the complex, old-school DICOM networking stack.
These services are the new building blocks for modern medical imaging:
- WADO-RS (Web Access to DICOM Objects – RESTful Services): This is your "get" or "retrieve" service. It's what allows a web browser or mobile app to request and display DICOM images from a server. It’s the engine behind today’s zero-footprint DICOM viewers that run right in your browser—no software installation required.
- STOW-RS (Store Over the Web – RESTful Services): This is the "store" or "upload" function. It provides a straightforward, web-based way to send DICOM files to a PACS or cloud archive. For example, a doctor could use a mobile app to snap a clinical photo, wrap it in a DICOM structure, and securely send it to the patient's record using STOW-RS.
- QIDO-RS (Query based on ID for DICOM Objects – RESTful Services): This is the powerful "search" tool. It lets an application find specific studies in an archive by querying for patient name, study date, or other metadata, all through a simple web request.
While the original DICOM protocol was built for TCP/IP transport, these RESTful services made it web-friendly. By using standard HTTP/HTTPS ports, DICOMweb allows for seamless integration with browsers and mobile devices, directly fueling the growth of telemedicine and remote care. As you can find out more on this topic, this initiative has unlocked a new level of flexibility in how we access imaging data.
Why This Evolution Matters for Modern Healthcare
This move to DICOMweb isn't just a technical footnote; it’s a strategic shift that supports the future of medicine. By making medical images available through standard web protocols, DICOMweb directly enables some of the most important trends in healthcare today.
Key Takeaway: DICOMweb doesn’t replace the original DICOM standards; it extends them. It acts as a bridge, connecting the robust, established world of PACS and modalities with the flexible, accessible world of the web and the cloud.
The implications are huge. A specialist can now review an urgent MRI from their tablet at home instead of racing to the hospital. Research institutions can build massive, cloud-based libraries of anonymized images to train AI models, pulling data securely through DICOMweb APIs. This evolution ensures that the DICOM standards remain the essential backbone of medical imaging, perfectly positioned to power a more connected and intelligent healthcare future.
Confronting Critical DICOM Security Vulnerabilities
In healthcare, protecting patient data isn’t just a best practice—it's a core ethical and legal duty. While DICOM is brilliant at making medical imaging devices talk to each other, the standard was born in a much simpler time, long before today’s sophisticated cyber threats were a daily reality. This history creates some serious security gaps we have to close.
Think about it: many older systems using DICOM were built to operate exclusively inside a hospital's trusted, private network. Because of this, features like native encryption and strong user authentication weren't always seen as must-haves. The alarming result is that, by default, DICOM traffic often sends sensitive Protected Health Information (PHI) as plain text, wide open for interception if the network is ever breached.
This isn't just a theoretical risk. The danger of unsecured DICOM is very real and has been proven time and again. A global scan of internet-connected radiology archives discovered a staggering 2,774 unprotected DICOM servers. Even more concerning, 719 of these were completely open, allowing anyone to access patient data without needing a password or dealing with any encryption. This shows just how easily even a modern hospital can accidentally expose its most sensitive information.
Putting Strong DICOM Security into Practice
The good news is that the DICOM standard does include security provisions. The challenge is making sure they are actually turned on and configured correctly. Securing imaging data requires a defense-in-depth strategy, layering protections at the network, application, and data levels.
One of the most effective moves you can make is to enforce encryption for all data on the move. You can do this by setting up DICOM over Transport Layer Security (TLS). This is the same workhorse encryption protocol that secures your online banking and shopping, and it wraps all DICOM communications in a secure, encrypted tunnel, making the data unreadable to anyone who might be snooping.
Beyond direct encryption, a few other network defenses are absolutely essential:
- Virtual Private Networks (VPNs): A VPN adds another powerful layer of encryption, which is especially important when clinicians need remote access or when teleradiology sends images over public internet connections.
- Firewalls and Access Control: Well-configured firewalls are your gatekeepers. They are critical for blocking access to DICOM ports and ensuring that only authorized devices and applications can connect to your PACS and imaging equipment.
Protecting Patient Data Beyond the Network
Your security job isn't done once the network is locked down. Protecting the data itself is equally important, especially when it’s repurposed for things like research, clinical training, or developing new software.
Key Strategy: Data anonymization is your most powerful tool for reducing risk. Before any imaging data is used for secondary purposes like training an AI model, all identifying patient information must be scrubbed from the DICOM headers.
This de-identification process means removing or replacing the 18 specific identifiers required by HIPAA, including the patient's name, birth date, and medical record number. On top of that, regular security audits are simply non-negotiable. These audits help you spot misconfigurations, outdated software, and other weak points before an attacker does.
Ultimately, securing DICOM systems is a continuous cycle of vigilance. For those developing medical software, looking into secure code integration and DevSecOps practices provides a roadmap for building security in from the start. By combining modern security protocols with disciplined data handling, healthcare organizations can keep reaping the benefits of DICOM while upholding their fundamental duty to protect patient privacy.
How DICOM Fuels the Future of Medical AI
Artificial intelligence is quickly graduating from a research concept to a real, practical tool in the radiologist's daily work. The engine driving this shift? The DICOM standard. The power of any AI comes from its ability to spot patterns in massive datasets, and DICOM files are so much more than simple pictures—they're perfectly structured, data-rich packages just waiting for analysis.
Think about it this way. If you wanted to teach an AI to recognize different car models, you wouldn't just show it random photos. You’d give it images carefully labeled with the make, model, year, and engine size. That context is what allows the AI to actually learn.
DICOM provides exactly this kind of rich context for medical imaging. Every .dcm file is essentially a pre-packaged training set, holding not just the pixels but a goldmine of metadata. This information, from patient history to the exact scanner settings used, is the high-octane fuel for modern medical AI.
Turning DICOM Data into AI-Driven Insights
The journey an AI model takes from raw data to a useful clinical insight is a well-defined path, and the DICOM standard acts as the guardrails every step of the way. This framework ensures data is handled consistently, securely, and in a way that makes sense for real-world clinical use.
Any serious AI pipeline in a medical setting has several key stages, all orchestrated using DICOM protocols. This structure is what makes building reliable and effective diagnostic tools possible in the first place.
Key Insight: DICOM is the essential bridge between the clinic and the world of AI development. It standardizes not just the input for AI models but also the output, making sure that AI-generated findings can slide right back into the patient's record without a hitch.
This complete, end-to-end integration is what elevates medical AI from a cool research project to a practical tool. Without the shared language of DICOM, the entire process would devolve into a chaotic mess of incompatible formats and communication breakdowns.
A Step-by-Step Look at a DICOM-Powered AI Workflow
The process of training and deploying a medical AI model isn't magic; it's a methodical procedure that leans heavily on DICOM’s structure. It’s all about getting the right data to the right place, securely and efficiently.
Here’s a simplified breakdown of how it typically plays out:
- Data Retrieval: It all starts with a query to the hospital’s Picture Archiving and Communication System (PACS). Using DICOM network commands like C-FIND and C-MOVE, researchers can pull thousands of relevant studies—for instance, every chest CT scan that might contain a lung nodule.
- De-identification: This is a non-negotiable security step. To protect patient privacy, all data must be anonymized before it’s used for training. This means scrubbing the DICOM headers of all 18 HIPAA-defined patient identifiers, like names, birth dates, and medical record numbers. The crucial image data stays, but the personal link is severed.
- Model Training: The now-anonymized DICOM files are fed into a machine learning model. The model chews through both the pixel data and the remaining metadata (like the scanner model or exposure settings) to learn the incredibly subtle patterns associated with a disease.
- Integrating AI Results: So, the AI model has found something—it's identified a suspicious lesion or calculated a tumor's volume. Now what? That result needs to get back to the clinician in a useful way. This is where DICOM's flexibility really shines.
The AI-generated insights are packaged into a new, special DICOM-compliant object. A very common format for this is DICOM Structured Reporting (DICOM-SR). This object can hold text, measurements, on-screen annotations, or even direct links to the specific frames in the original scan.
Because this report is itself a DICOM object, it can be sent back to the PACS with a simple C-STORE command and stored right alongside the original images. The radiologist can then see the AI's findings directly inside their everyday DICOM viewer, fully integrated into their workflow. It's this seamless feedback loop that makes DICOM the true launchpad for the next generation of AI-powered medicine.
Got Questions About DICOM? Let's Clear Things Up.
Diving into medical imaging, you'll inevitably bump into some common questions about DICOM. It's a foundational standard, but some of its concepts can feel a bit tangled at first. This section is all about untangling them.
Think of this as a quick, practical Q&A session where we tackle the most frequent points of confusion and give you the straightforward answers you need.
What's the Real Difference Between DICOM and PACS?
This is easily the most common question, and it's a great one because the two are so intertwined. The best way to think about it is with a simple analogy: DICOM is the "language," and PACS is the "library."
DICOM is the universal set of rules—the format for the files, the protocols for sending them, the structure of the data. It's the shared grammar that lets an MRI scanner in Germany "talk" to a viewing workstation in Brazil. Without it, every machine would be speaking a different dialect, and chaos would ensue.
A PACS (Picture Archiving and Communication System), on the other hand, is the actual technology that uses that language. It's the massive digital archive—the servers, software, and workstations—that a hospital uses to store, organize, find, and display millions of medical images. It's the building that houses all the books.
Key Takeaway: A PACS can't function without DICOM. It would be like a library with no cataloging system and books in a thousand different languages. DICOM provides the essential rules, and the PACS provides the infrastructure to put those rules into action.
They have a symbiotic relationship. You absolutely need the standard (DICOM) to ensure everything is compatible, and you need the system (PACS) to handle the immense volume of daily imaging data.
Is a DICOM File Just a Fancy JPEG?
Not even close. While you can technically save the image portion of a DICOM file as a JPEG, doing so strips out nearly everything that makes it medically and legally useful. A regular image file, like a JPEG or PNG, is just that—a picture. It contains pixel data and nothing more.
A DICOM file is a much smarter, more complete package. It's a container that bundles two inseparable things:
- The image itself, often stored with lossless compression to make sure every single diagnostic detail is perfectly preserved.
- A huge header of metadata, which is the file's DNA. This includes everything from the patient's name and ID to the exact voltage and exposure time used by the scanner.
This attached data isn't just nice to have; it's critical. It creates a complete, auditable record that gives a radiologist the context they need to make an accurate diagnosis. Converting a DICOM file to a JPEG is like ripping the first 20 pages out of a patient's chart—you're left with some information, but you've lost the vital context that gives it meaning.
How Can I Open a DICOM File on My Computer?
If you've ever tried to double-click a .dcm file, you've probably noticed that your computer's built-in photo app has no idea what to do with it. That’s because these apps are designed to see pixels, not the rich, structured metadata that is the heart of the DICOM standards.
To look at a DICOM file correctly, you need a dedicated DICOM viewer. These are special programs built to understand both the image and all the attached header data.
The good news? You don't have to work in a radiology department to get one. There are many excellent, free DICOM viewers perfect for personal or educational use. A few popular choices include:
- RadiAnt DICOM Viewer (for Windows)
- MicroDicom (also for Windows)
- Horos (a go-to for macOS users)
These viewers let you see the image and poke around in the metadata, giving you a real sense of just how much information is packed into one of these files. In a clinic, radiologists use high-end, commercial PACS workstations, but they are all built on the same fundamental principle of being DICOM-compliant.
Are DICOM Standards Still Relevant with AI and the Cloud?
Absolutely. In fact, DICOM is more critical now than ever before. Far from becoming a relic, the standard has smartly evolved to become the bedrock for modern medical technology.
The biggest game-changer here is the DICOMweb initiative. This update created a set of RESTful web services that let imaging data be accessed securely over the internet using the same web protocols that power the rest of the digital world.
This was the key that unlocked the future of medical imaging:
- Cloud-based PACS: It allows hospitals to shift their gigantic image archives to the cloud, slashing on-site infrastructure costs and making data accessible from anywhere.
- AI-driven analysis: AI companies can build platforms that securely pull anonymized imaging data from multiple hospitals to train and test diagnostic algorithms on a massive scale.
- Mobile viewing: It empowers doctors to review a patient's CT scan securely on a tablet, whether they're in another part of the hospital or another country.
So, instead of being pushed aside by new tech, DICOM adapted. It has solidified its position as the essential data backbone connecting traditional radiology with the future of intelligent, connected healthcare.
At PYCAD, we live and breathe DICOM. We specialize in using the power of these standards to build and deploy sophisticated AI solutions for medical imaging. From anonymizing and annotating data to training models and deploying them via API, we help medical device companies accelerate their innovation pipeline.
See how our expertise can bring your medical AI projects to life by visiting us at https://pycad.co.






