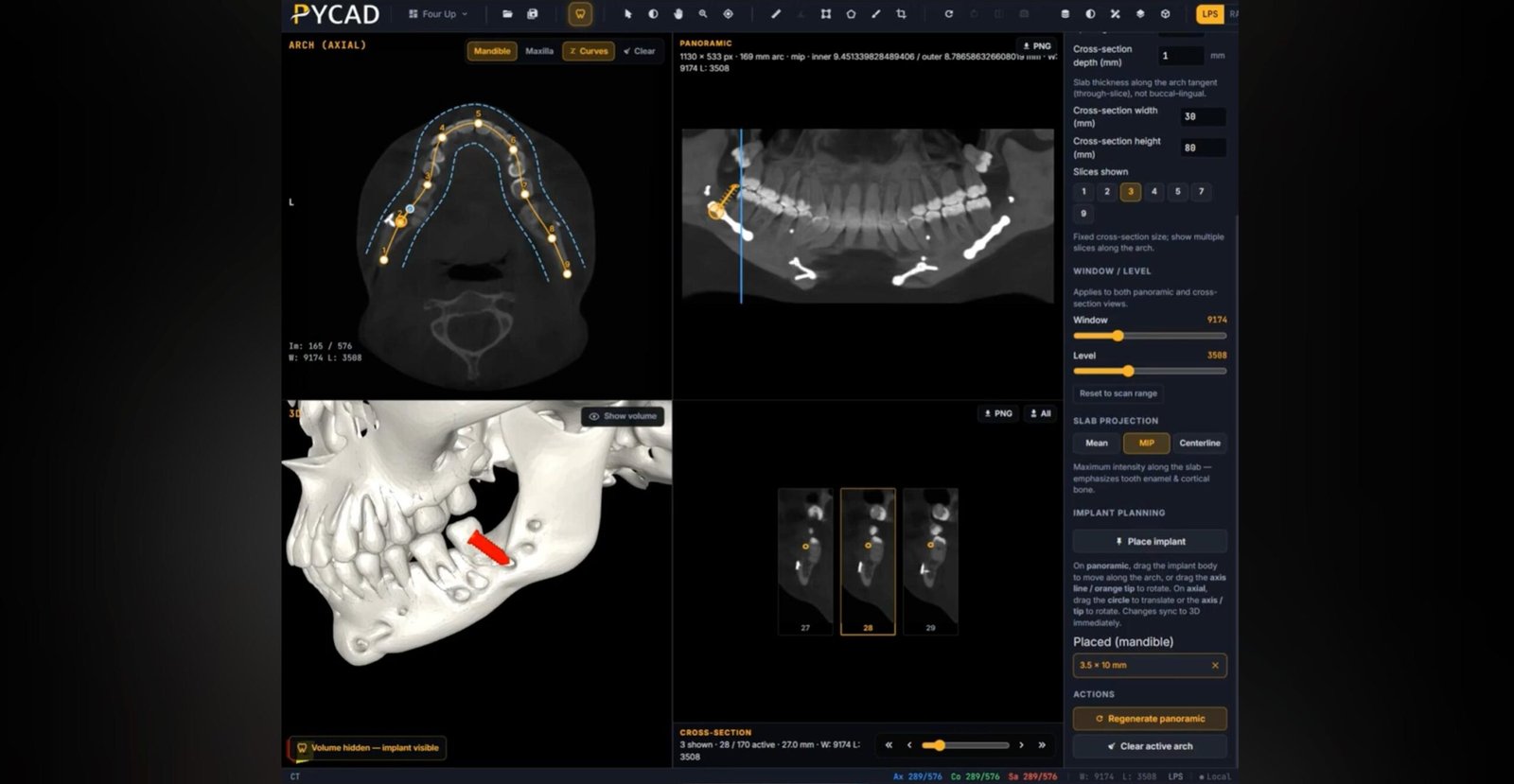
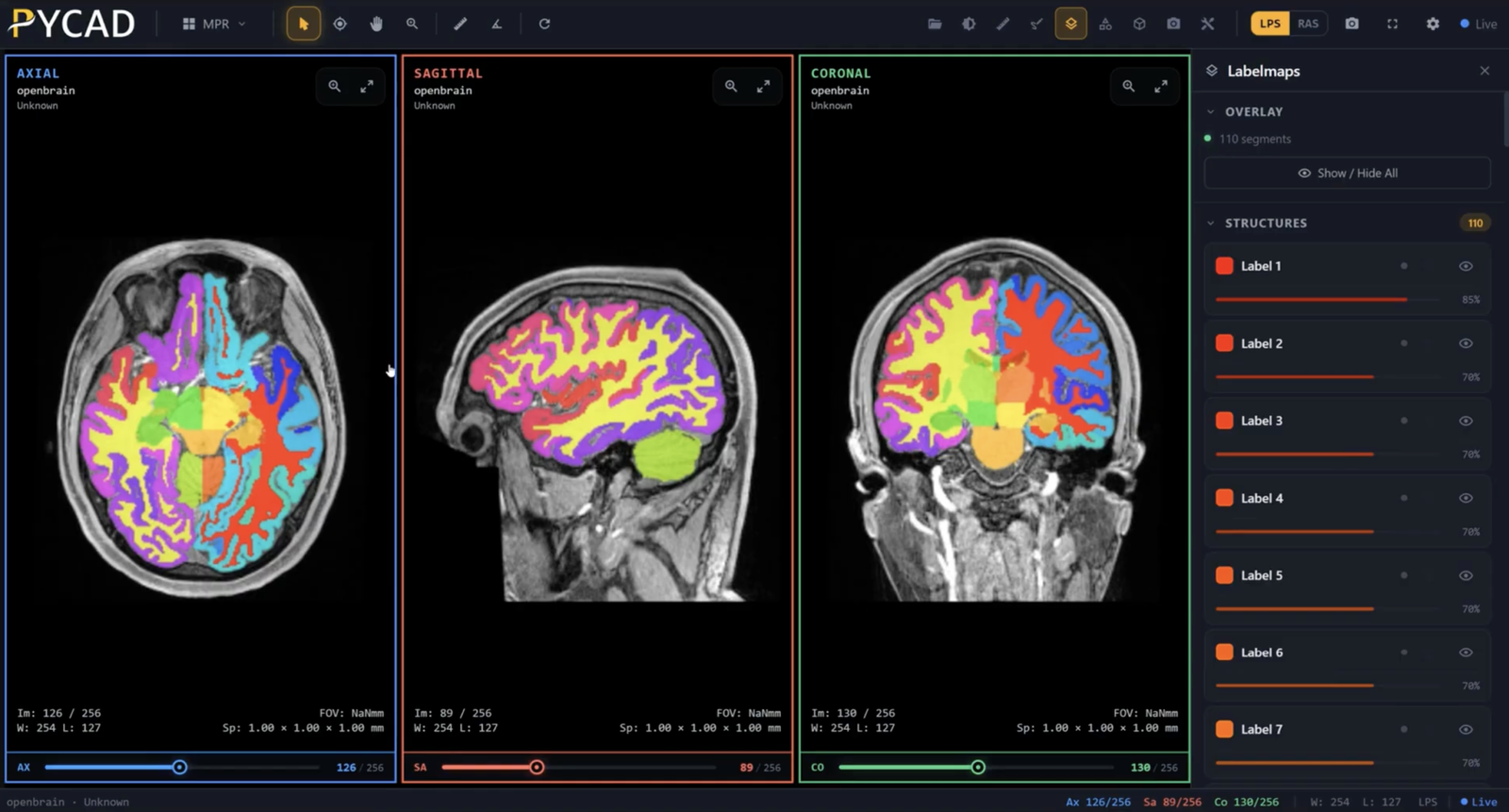
Ever tried to open a file on your computer only to find out you don't have the right software? It's frustrating. Now, imagine that file is a life-saving CT scan, and the inability to open it could delay a critical diagnosis. That's the chaotic world medical imaging lived in before the DICOM standard.
DICOM, which stands for Digital Imaging and Communications in Medicine, is essentially the universal language of medical imaging. It's the reason an MRI scanner from one manufacturer can send an image that a radiologist can instantly view on a workstation made by a completely different company. It acts as a digital Rosetta Stone, ensuring seamless communication across the entire healthcare ecosystem.
Why DICOM Is the Bedrock of Medical Imaging
Let's rewind to a time before DICOM became the industry norm in the 1990s. Medical device manufacturers all used their own proprietary file formats. This created closed-off ecosystems, effectively locking hospitals into a single vendor. If you bought a GE scanner, you needed a GE workstation to view the images. Sharing that scan with a hospital using Siemens equipment? Good luck.
This created dangerous information silos. A patient’s vital diagnostic data was often stuck at the facility where it was created, making it incredibly difficult to get second opinions, consult with specialists, or even switch hospitals without redoing expensive and time-consuming scans. DICOM was created to tear down these walls.
The Power of a Universal Language
At its heart, DICOM achieves interoperability by standardizing two fundamental components:
- A Unified File Format: It dictates a precise structure for how an image file is built. This isn't just the pixel data; it also includes a rich header packed with crucial patient metadata—like their name, ID, the date of the scan, and even the specific scanner settings used.
- A Common Network Protocol: It defines the rules for sending and receiving these files over a network. Think of it like the postal service for medical images; it provides a reliable system to ensure a scan sent from a CT machine arrives intact at the radiologist's review station or the hospital's central archive.
By tackling both the file and its transmission, DICOM ensures that every compliant device, from ultrasound machines to advanced imaging archives, speaks the same clinical dialect.
DICOM is far more than a technical specification; it's a framework for collaboration. It empowers specialists to share vital patient images and data effortlessly, which is absolutely fundamental to accurate diagnosis, effective treatment planning, and modern team-based medicine.
Impact on Clinical Efficiency and Patient Care
The real-world benefits of this standard are profound. Because of DICOM, a patient's complete imaging history can follow them wherever they go, creating a comprehensive medical record that is accessible to any authorized provider.
This seamless flow of information has a direct, positive impact on day-to-day care. When a trauma patient arrives in the ER, doctors can pull up prior X-rays from an outpatient clinic in seconds to assess new injuries. An oncologist can compare a new PET scan against one from six months ago to precisely track a tumor's response to treatment.
This isn't just about convenience. This level of efficiency accelerates decision-making, boosts diagnostic accuracy, and ultimately leads to better patient outcomes. In this guide, we'll dive deeper into the components and best practices that make the DICOM standard so indispensable to modern healthcare.
Understanding the Core Pillars of DICOM
To really get a handle on how DICOM brings order to the complex world of medical imaging, you need to understand its three main parts. These components work together to make sure that an image taken on one machine can be reliably stored, sent across a network, and understood by a completely different piece of equipment, even if they're from competing manufacturers.
Think of it this way: if you're sending a sensitive package, you need three things. You need the package itself (the file), a reliable courier service that knows how to handle it (the network protocol), and a clear shipping label stating what's inside and where it's going (the conformance statement). DICOM provides all three for medical images.
The standard didn't just appear overnight. It has evolved significantly over the years, adapting to new technologies and clinical needs. This infographic provides a great visual overview of its journey.
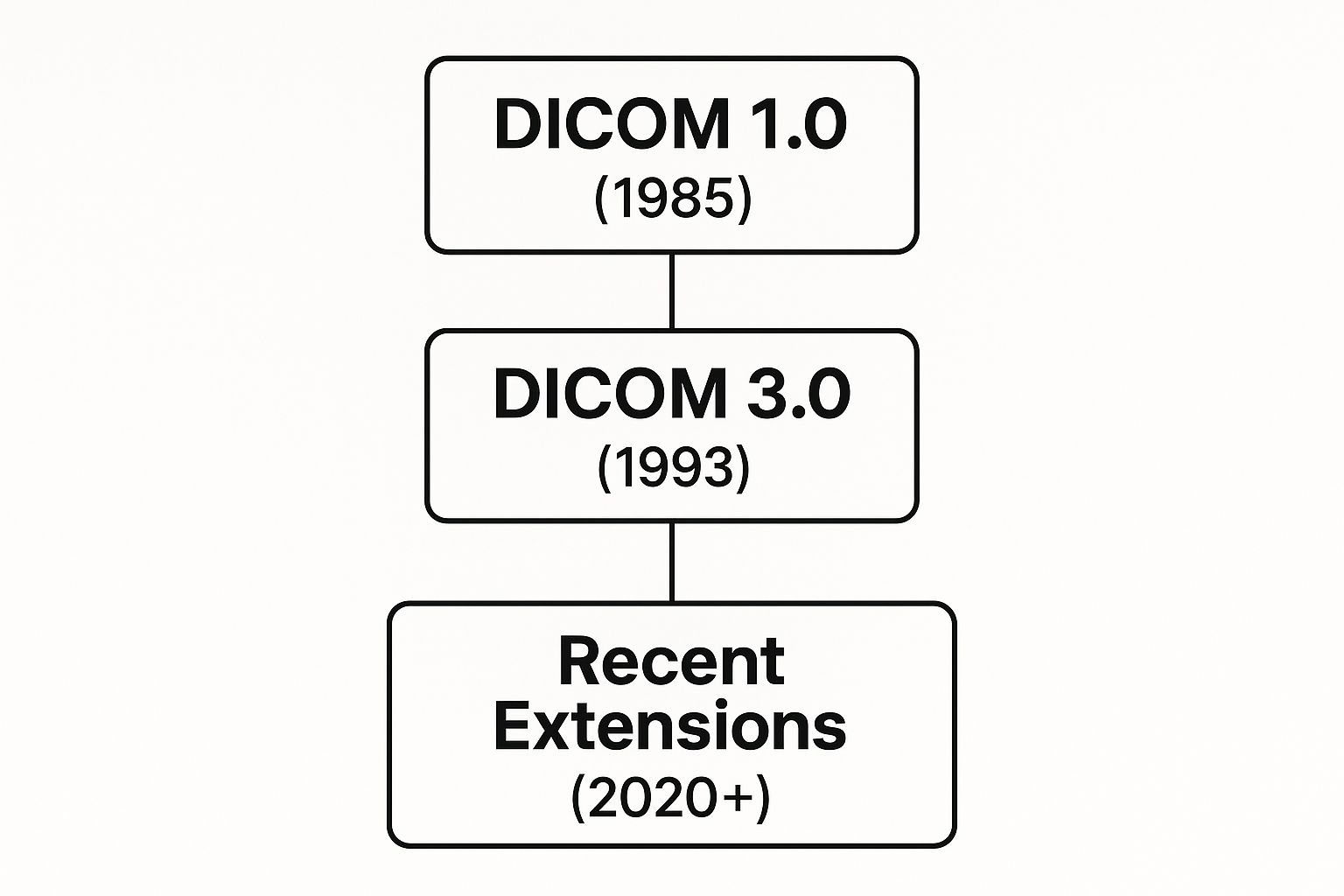
As you can see, the release of Version 3.0 in 1993 was a pivotal moment, laying the foundation for the interconnected system we rely on today.
To break it down further, let's look at each of DICOM's three pillars and the practical role they play in a healthcare setting.
| Component | Primary Function | Real-World Analogy |
|---|---|---|
| File Format | Stores the image and its associated metadata in a single, standardized package. | A detailed patient file folder, containing not just a photo but all the notes, lab results, and identification attached to it. |
| Network Services | Defines the "language" and commands for devices to communicate and transfer data over a network. | A specialized, secure courier service (like FedEx for medical data) with specific instructions for sending, finding, and retrieving packages. |
| Conformance Statement | A technical document from a manufacturer detailing exactly which DICOM functions a device supports. | A device's professional resume or API documentation, clearly stating its communication skills and limitations for potential employers (the hospital's IT team). |
Each of these pillars solves a unique problem, and without all three working in harmony, the seamless exchange of medical images that clinicians depend on would fall apart.
The DICOM File Format Itself
First up is the file format. Calling a DICOM file just an "image" is a massive understatement. It's really a sophisticated, self-contained data container.
Every DICOM file is built from two core parts:
- Pixel Data: This is the visual image you see—the X-ray, the CT slice, or the ultrasound video.
- Metadata Header: This is a rich, structured block of text-based information that is permanently attached to the pixel data.
This metadata is the secret sauce. It includes everything from the patient's name and ID to the exact scanner settings used, the date and time of the exam, and even notes from the technologist. This ensures that an image never loses its clinical context, which is absolutely critical for preventing dangerous mix-ups and ensuring accurate diagnosis.
DICOM Network Services
The second pillar is the set of network services, often called DICOM Messaging or, more technically, DIMSE (DICOM Message Service Element). If the file format is the letter, then DIMSE is the specialized postal service that knows exactly how to deliver it. These services are a list of commands that DICOM-compliant devices use to talk to each other over a network.
For instance, when an MRI machine completes a scan, it uses a DIMSE command called C-STORE to push the images to a Picture Archiving and Communication System (PACS) for long-term storage. Later, a radiologist at a viewing workstation might use another command, C-FIND, to search the PACS for that patient's previous studies.
These network protocols are the active-duty workhorses of the DICOM standard. They are the commands that tell systems to push, pull, find, and move imaging data throughout a hospital's network, creating a dynamic and responsive workflow.
The DICOM Conformance Statement
The final piece of the puzzle is the DICOM Conformance Statement. This is a crucial, though often overlooked, technical document that every manufacturer must provide for their equipment. It's best to think of it as a device's resume—a detailed summary of its communication capabilities.
This document clearly lists which DICOM services and file types the device can handle. A simple portable ultrasound, for example, might only support the C-STORE service to send images out. An advanced radiology workstation, on the other hand, will support a whole suite of services for searching (C-FIND), retrieving (C-MOVE), and even printing (N-PRINT).
Before a hospital invests in a new CT scanner, the IT department will scrutinize its Conformance Statement. Why? To guarantee the new machine can "speak the same language" as their existing PACS and other imaging systems. This step is essential for preventing expensive integration headaches and ensuring true interoperability between devices from different vendors.
The Global Journey of the DICOM Standard
DICOM didn’t just materialize out of thin air. It was forged from necessity, born out of the digital chaos that defined early medical imaging. Picture the scene in the early 1980s: every CT or MRI scanner manufacturer had its own unique, proprietary image format. This was a nightmare for hospitals. It locked them into a single vendor's ecosystem, making it a Herculean task to share crucial diagnostic images between departments, never mind with other facilities. These data silos were creating serious, and frankly, dangerous, bottlenecks in patient care.
Something had to give. Recognizing the urgency, the American College of Radiology (ACR) and the National Electrical Manufacturers Association (NEMA) teamed up. Their mission was straightforward but incredibly ambitious: create a single, unified standard for storing and transmitting medical images. This collaboration gave us the first version of the standard in 1985, but the real turning point came in 1993 with the release of Version 3.0.

From Radiology to a Global Benchmark
Version 3.0 wasn't just an update; it was a complete overhaul. It was the first time the standard was officially called "DICOM," and more importantly, it was engineered to operate over standard computer networks using TCP/IP protocols—the very same backbone that runs the internet. This was a monumental shift. DICOM was no longer just about connecting specific pieces of hardware; it had become a globally scalable software solution.
This release also dramatically broadened its horizons. While radiology was the original catalyst, Version 3.0 was designed to support a much wider spectrum of medical imaging.
The effect was immediate and far-reaching. The standard quickly evolved to meet the specific demands of other specialties, such as:
- Cardiology: Managing dynamic data from echocardiograms and angiograms.
- Pathology: Supporting the massive files generated by whole-slide imaging.
- Endoscopy: Handling video feeds captured during internal procedures.
- Surgery: Integrating real-time images and videos straight from the operating room.
This expansion proved that the core principles of the DICOM standard were robust and flexible enough to serve as a universal backbone for nearly all forms of medical imaging, cementing its value across the entire healthcare enterprise.
Worldwide Adoption and Collaborative Growth
The true testament to DICOM's success is its global embrace. The standard was built for interoperability, and the world took notice. By the mid-1990s, international standards bodies were getting on board. For instance, Europe’s CEN TC 251 adopted it as their MEDICOM standard, while Japan’s MIPS standard was based heavily on DICOM. This wave of international adoption, eventually involving contributions from over a dozen global organizations, highlighted the universal need for a common language in medical imaging.
Understanding this history is more than just a trivia lesson; it explains why DICOM is so deeply woven into the fabric of modern healthcare. Its journey from a niche radiology solution to a global, multi-specialty powerhouse is a story of collaborative design and relentless adaptation. This legacy of evolution is what keeps it relevant today, providing a stable foundation for the next wave of innovation—including the integration of AI into our clinical workflows.
Keeping Patient Data Safe in DICOM Systems
The very thing that makes DICOM so powerful—its ability to let different medical devices and systems talk to each other seamlessly—is also what can make it vulnerable. Think about it: a system built for easy sharing can, without the right precautions, become an open door for the wrong people. The ability to send a CT scan across a hospital network in seconds is a modern marvel, but that same pathway has to be locked down tight to protect patient privacy.
The real challenge is striking the right balance between making data accessible to doctors who need it and keeping it confidential from everyone else. Often, the biggest security holes aren't sophisticated hacks but simple mistakes, like leaving a server unprotected or a network wide open. This can expose entire archives of patient data. For any healthcare IT team, the job is clear: build a DICOM network that's both fast and fundamentally secure.
Where Are the Weak Spots?
This isn't just a theoretical problem. When you look at how DICOM is used in the real world, the security gaps become painfully obvious. Even though the standard has been around for decades, its implementation has hit some serious security snags.
A 2016 study that scanned the internet for open DICOM servers found some shocking numbers. Researchers discovered 2,774 unprotected servers worldwide. Even more alarming, 719 of those were completely open, meaning anyone could access the patient data inside without any credentials at all. This wasn't just happening in small clinics; major hospitals in developed countries had huge security holes, putting vast amounts of sensitive imaging data at risk.
This just goes to show that you can't be passive about cybersecurity. Healthcare organizations have to get proactive and build security into their systems from the ground up, not just as an afterthought.
The goal of easy data sharing can never be more important than patient privacy. A truly effective DICOM environment lets data flow freely to the right clinicians but remains completely sealed off from outside threats.
Best Practices for Locking Down Your DICOM Infrastructure
Securing a DICOM environment isn’t about finding one magic bullet. It’s about creating layers of defense that protect data at every stage, from the imaging machine to the long-term archive. Here are the essential steps every healthcare facility should take.
1. Control Who Gets Access
Not everyone in a hospital needs to see every patient's scans. The first line of defense is role-based access control (RBAC). This simple but powerful principle ensures that a radiologist can view and analyze images, but a billing administrator can't. It's common sense: limit access to only what's necessary for someone's job. This not only stops prying eyes inside the organization but also minimizes the damage if a user's account is ever compromised.
2. Encrypt Everything, Everywhere
Data is at risk in two main states: when it's moving across a network (in transit) and when it's sitting on a server (at rest). You have to protect it in both places.
- For data in transit: Use secure communication protocols like Transport Layer Security (TLS) for all DICOM traffic. This wraps the data in an encrypted tunnel as it travels between devices, making it unreadable to anyone trying to eavesdrop on the network.
- For data at rest: Any data stored in a PACS or other archive must be encrypted. That way, even if a physical server is stolen or a cloud storage bucket is breached, the patient files themselves remain scrambled and useless to the thief.
3. Run Regular Security Check-ups
You can't defend against a threat you don't know about. That's why regular, thorough security audits are an absolute must. These aren't just box-ticking exercises; they involve actively looking for weaknesses through vulnerability scans, penetration testing, and reviewing who has accessed what data. This process helps you find and fix security holes before they can be exploited, keeping your entire medical imaging ecosystem safe.
How DICOM Standards Power Medical AI

The incredible rise of artificial intelligence in medicine isn't just about clever algorithms—it's built on a foundation of high-quality data. AI models, especially those used for diagnostics, are incredibly data-hungry. To learn how to spot a tumor or identify a fracture, a model has to train on thousands, sometimes millions, of example images. This is where DICOM standards go from being a simple file format to the essential fuel for medical innovation.
Think about it this way: you wouldn't get very far trying to teach an AI to recognize cats by feeding it a random jumble of blurry photos, kids' drawings, and professional portraits, all with different or missing information. The results would be a mess. Medical AI faces the exact same problem. For any machine learning model to be effective and safe, it needs clean, consistent, and context-rich data.
DICOM provides that exact structure. Because every DICOM file is standardized, AI developers can build reliable data pipelines that feed models with uniform images. Even more importantly, they can use the wealth of metadata baked into each file to guide the learning process.
Training AI with Structured DICOM Data
The metadata inside a DICOM file is a genuine goldmine for training AI. An algorithm doesn't just see a picture of a lung. It sees a CT slice of a lung from a specific patient, taken on a particular date with a GE scanner using precise exposure settings. That context is absolutely critical.
This structured information lets data scientists:
- Filter Datasets: They can effortlessly pull all chest CT scans from male patients over 60 to train a model for a very specific demographic.
- Normalize Images: Information about scanner settings helps algorithms account for subtle differences between machines, making the final model more accurate.
- Provide Ground Truth: Labels and annotations can be programmatically tied to specific studies, teaching the AI what to look for with pinpoint accuracy.
Think of DICOM metadata as the perfect set of labels for a vast digital library. It tells the AI not just what is in the image, but also the who, when, where, and how. This structured context is fundamental for building diagnostic tools that are both powerful and trustworthy.
This whole process turns a simple image archive into a high-value training ground. AI can begin to learn the subtle patterns of disease across thousands of cases, picking up on markers that might be invisible to the human eye.
Integrating AI into Clinical Workflows
Of course, a brilliant AI model is useless if it can't fit smoothly into a clinician's daily routine. Once an AI is trained, DICOM standards again play a huge role in its deployment. The results of an AI analysis—say, a highlighted nodule on a scan or a calculated risk score—have to be sent back into the clinical environment.
This is often done by creating new DICOM objects. For example, an AI tool might generate a DICOM Structured Report with its findings or create a DICOM Presentation State that overlays a heatmap onto the original image to flag areas of concern. Because these outputs stick to DICOM standards, they are instantly compatible with the hospital’s existing PACS and physician workstations. A radiologist can see the AI's analysis right next to the original scan without juggling special software.
This built-in interoperability ensures that AI acts as a helpful assistant, not a disruptive new technology. It slots directly into the established workflow, augmenting the radiologist's expertise instead of trying to upend it. As DICOM continues to shape medical AI, it's also interesting to see how broader innovations like Nocode Backend AI solutions are making it easier to build machine learning applications that can interact with this kind of complex medical data.
The standard itself is also evolving. New workgroups are actively focused on creating specific DICOM objects for AI results, making sure that machine learning outputs can be stored, sent, and displayed in a standardized way. This is clear proof that DICOM isn't some dusty legacy format; it’s an active, critical catalyst for the future of AI in medicine.
The Future and Reach of DICOM Today
After decades of hard work and global cooperation, the DICOM standard isn't just a success story; it's the very foundation of modern medical imaging. Its presence is so woven into the fabric of healthcare that trying to operate without it is practically unimaginable. DICOM’s current reach is a powerful testament to its smart design and the universal problem it was built to solve.
Today, DICOM is the default language spoken by nearly all medical imaging equipment and healthcare IT systems. Whether you're in a massive research hospital or a small community clinic, the devices from every major manufacturer are communicating using DICOM. This isn't limited to just one area—it covers every modality, from CT and MRI scans to complex cardiology imaging. In fact, manufacturers are required to publish a conformance statement, a document that spells out exactly which DICOM services their equipment supports, which keeps everyone honest and ensures things actually work together.
Beyond the Hospital Walls
While its heart is in clinical medicine, DICOM's flexible nature has allowed it to find a home in some surprising places. The core concept—bundling complex visual data with rich, structured metadata—has proven incredibly valuable far beyond patient care. It shows that DICOM isn't some dusty old protocol but a living standard that continues to adapt.
For instance, DICOM is now being used in:
- Digital Pathology: To manage the massive whole-slide images needed to diagnose diseases from tissue samples.
- Airport Security: To standardize data from advanced luggage scanners, helping to improve threat detection.
- Industrial Testing: To inspect critical parts like jet engines or oil pipelines for tiny flaws using non-destructive testing (NDT) methods.
Seeing DICOM pop up in these other high-stakes fields really highlights the power of a well-designed, universal standard for imaging data.
Evolving for a Connected Future
The people steering the DICOM standard know that technology never sits still. To stay relevant, DICOM has kept evolving, especially to meet the modern need for web and mobile access. This led to the creation of DICOMweb, a set of RESTful services that use familiar web technologies like HTTPS to make medical images available anywhere, on any device.
You can think of DICOMweb as a bridge connecting the secure, traditional hospital network to the flexible world of cloud computing and mobile health. It’s what allows a radiologist to securely pull up a critical scan on a tablet from home—a scenario that would have seemed like science fiction not long ago.
This forward-thinking approach is exactly what will keep DICOM essential for years to come. It has gracefully shifted from a solution for a 1980s problem to the backbone for 21st-century imaging. Far from being obsolete, the DICOM standard is the resilient and indispensable engine driving the future of imaging worldwide.
Frequently Asked Questions About DICOM
Even after getting a good handle on the DICOM standard, a few common questions always seem to pop up. Getting straight answers to these helps connect the dots and clarifies how DICOM actually works in the real world.
What's the Difference Between DICOM and PACS?
This is easily one of the most common questions, and it gets to the heart of the difference between a standard and a system. The best analogy I've found is music.
Think of an MP3 as the standard file format for a song. Spotify, on the other hand, is the system you use to store, organize, and play those songs.
It’s the same relationship here:
- DICOM is the file format. It’s the universal structure for a medical image and all its associated data, bundled together.
- A PACS (Picture Archiving and Communication System) is the system. It’s the digital filing cabinet—the entire infrastructure of software and hardware that stores, finds, and manages all those DICOM files.
So, while a PACS is built to work with DICOM files, they are two separate but essential parts of the same ecosystem. You can't have a modern medical imaging workflow without both.
Is DICOM Only Used for Radiology?
Not at all. While radiology was certainly DICOM's origin story, its reach has expanded far beyond that. The standard was intentionally designed to be flexible, which has allowed it to grow and adapt to nearly every medical specialty that generates images.
Today, the DICOM standard is a cornerstone for a wide range of medical fields, including cardiology, pathology, dentistry, endoscopy, and even surgery. Its ability to handle different types of image data—from static X-rays to dynamic ultrasound videos—makes it a truly versatile tool across the entire healthcare enterprise.
This widespread adoption is a huge testament to the standard's robust and forward-thinking design.
Why Is a DICOM Conformance Statement Important?
A DICOM Conformance Statement is a critical technical document provided by a manufacturer for any piece of equipment. Honestly, it's non-negotiable for ensuring interoperability. Think of it as a device’s professional resume or a detailed list of the languages it speaks.
Before a hospital invests in a new MRI machine, the IT department will scrutinize its Conformance Statement. They need to confirm it can speak the same "language" as their existing PACS and workstations. The statement spells out exactly which DICOM services the machine supports, like storing, printing, or finding images.
This simple check prevents massive headaches and costly integration failures down the road, ensuring a new piece of equipment can slot right into the hospital's network without a hitch.
At PYCAD, we specialize in integrating AI directly into these complex medical imaging workflows. Our expertise in handling DICOM data ensures that AI models are not only powerful but also fully compatible with existing clinical systems. To see how our solutions can enhance your medical devices, explore our services.